Overview
The 2025 ADA guidelines bring forth significant updates designed to enhance diabetes management through personalized care strategies, improved technology integration, and a focus on emotional health. It's important to recognize that these updates emphasize the value of individualized treatment plans. For instance, recommending Continuous Glucose Monitoring for adults with Type 2 Diabetes can make a real difference. Additionally, incorporating emotional health screenings equips healthcare providers with the necessary tools to effectively support patients in managing their condition.
You're not alone in this journey. These updates are here to help you feel understood and supported. By focusing on your unique needs, healthcare providers can offer the personalized care you deserve. Remember, seeking help and resources is a vital step in managing your diabetes effectively. Together, we can navigate this path toward better health.
Introduction
In a world where diabetes management is continually evolving, the 2025 ADA Guidelines stand as a beacon of hope and innovation for patients and healthcare providers alike. These updated guidelines introduce a wealth of pivotal changes designed to enhance care through personalized strategies, advanced technology integration, and a holistic approach to health.
With a specific emphasis on individualized treatment plans, emotional well-being, and the incorporation of cutting-edge tools like Continuous Glucose Monitoring, the guidelines reflect a profound understanding of the complexities surrounding diabetes. It's understandable to feel overwhelmed by these changes, especially as the prevalence of diabetes, particularly among youth and older adults, continues to rise.
These guidelines serve as a critical resource for fostering better health outcomes and improving the quality of life for millions. The implications of these updates are far-reaching, offering both patients and providers a structured pathway to navigate the challenges of diabetes management effectively. Remember, you're not alone in this journey; we are here to support you every step of the way.
Overview of the 2025 ADA Guidelines
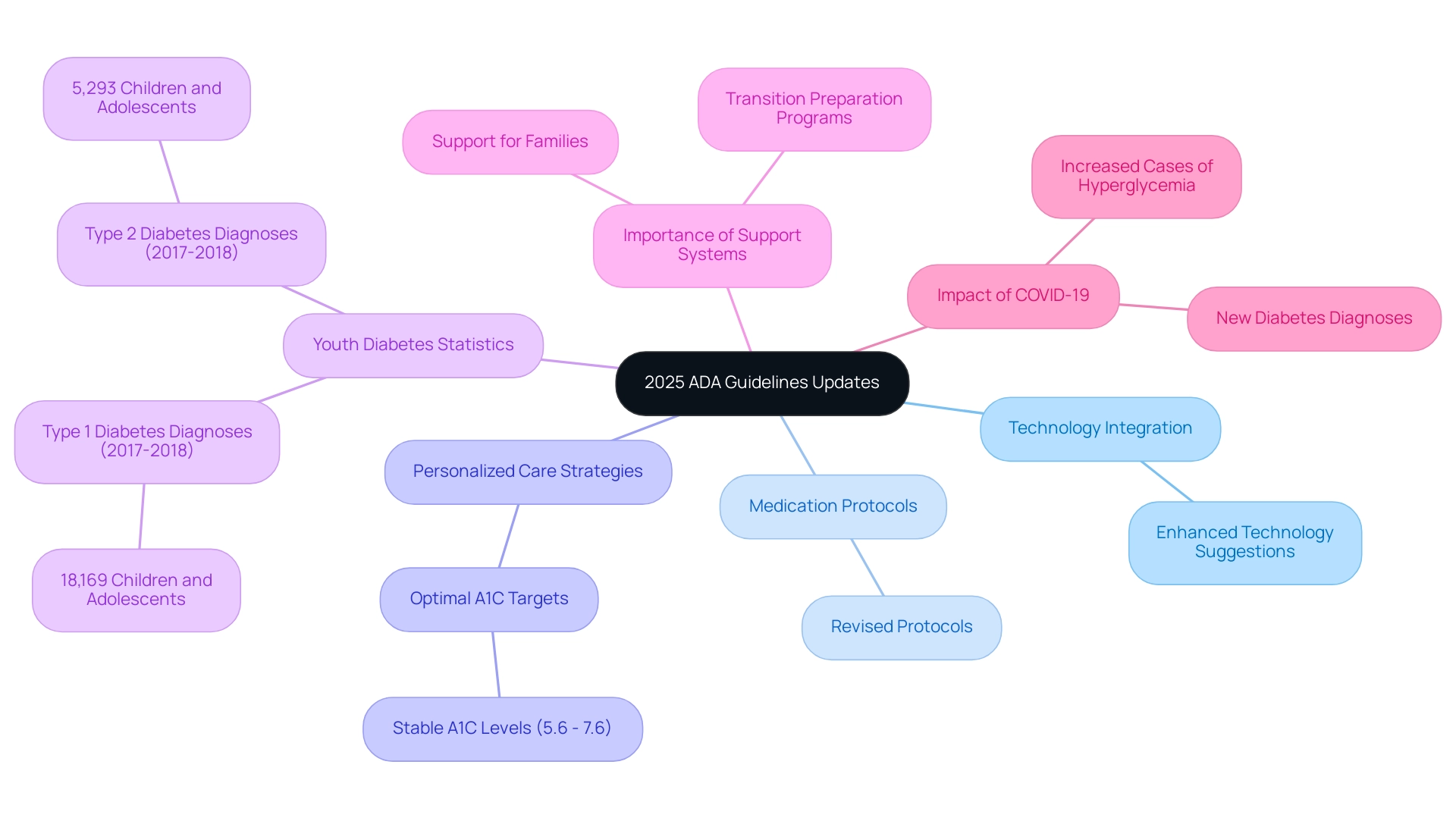
The updates in the ADA guideline 2025 are pivotal for improving diabetes management, and we understand how important this is for you. Among these updates are:
- Enhanced suggestions for integrating technology into management practices
- Revised medication protocols
- A strong emphasis on comprehensive well-being
These guidelines are based on the latest research and clinical practices, equipping healthcare providers with the most relevant information to effectively assist those they care for.
A notable aspect of this year's updates is the emphasis on personalized care strategies that consider the unique needs and circumstances of each individual. This approach aims to make managing blood sugar levels more accessible and effective for a diverse range of populations. For instance, stable A1C levels between 5.6% and 7.6% (38 to 60 mmol/mol) are now emphasized as optimal targets for many individuals, reflecting a tailored approach to personal health goals.
Additionally, the guidelines address the alarming rise in diagnoses of the condition among youth, with an estimated 18,169 children and adolescents diagnosed with type 1 and 5,293 with type 2 during 2017-2018. This trend underscores the critical need for early intervention and education, as well as the importance of transition preparation programs for youth moving from pediatric to adult healthcare. It’s understandable to feel concerned about this issue, and it is crucial to have comprehensive support systems for these young patients and their families.
The 2025 updates also incorporate expert opinions on the necessity of adapting care for blood sugar management to the evolving landscape shaped by factors such as the COVID-19 pandemic, which has been linked to increased cases of hyperglycemia and new diagnoses. As Charles "Chuck" Henderson, CEO, stated, "Enhancing the lives of individuals impacted by this condition is a key part of the ADA’s mission." The ADA provides the reliable assistance required for individuals living with the condition and those supporting them to manage the illness and flourish until a cure is discovered.
At T2D Solutions, we are dedicated to offering a comprehensive resource hub for individuals recently diagnosed with this condition. Our platform will provide educational resources, community assistance, and tools to help you navigate your health journey in light of the ADA guideline 2025. We encourage you to subscribe to our updates to stay informed about new resources and support available through T2D Solutions, ensuring you receive the comprehensive assistance you deserve.
Enhanced Recommendations for Continuous Glucose Monitoring in Type 2 Diabetes
The ADA guideline 2025 has introduced a pivotal recommendation: Continuous Glucose Monitoring (CGM) is now advised for adults with Type 2 Diabetes who are utilizing glucose-lowering medications other than insulin. This marks a revolutionary step forward in managing blood sugar levels. CGM technology offers real-time glucose information, empowering individuals to make informed choices about their diet, exercise, and medication modifications.
Research indicates that consistent use of CGM can significantly enhance glycemic control. Studies reveal a strong correlation between maintaining CGM usage for over 70% of the time during a 14-day period and improved mean glucose levels over three months. Moreover, CGM has been associated with a notable reduction in hypoglycemic events, underscoring its role as a critical tool in personalized care for those facing blood sugar challenges.
Real-world examples illustrate the effectiveness of CGM in improving A1C levels among individuals managing their blood sugar. For instance, a quality enhancement initiative highlighted the positive impact of CGM on decision-making and understanding health management, leading to improved health outcomes. As Lynne Kinson, the corresponding author of the program, noted, 'Continuous glucose monitoring in individuals with type 2 conditions: a quality enhancement initiative' emphasizes the importance of integrating CGM into treatment strategies.
Furthermore, T2DSolutions' focus on community support aligns with findings from the case study 'Community Building in Diabetes Care,' which shows how shared experiences can enhance care. Specialists in the field advocate for incorporating CGM into care plans, emphasizing its benefits in promoting proactive control strategies. The ADA guideline 2025 reinforces this by recommending CGM as a standard practice, reflecting a growing recognition of its value in enhancing the quality of life for individuals managing Type 2 Diabetes. You're not alone in this journey; we are here to support you every step of the way.
Expanded Role of GLP-1 Receptor Agonists in Diabetes Management
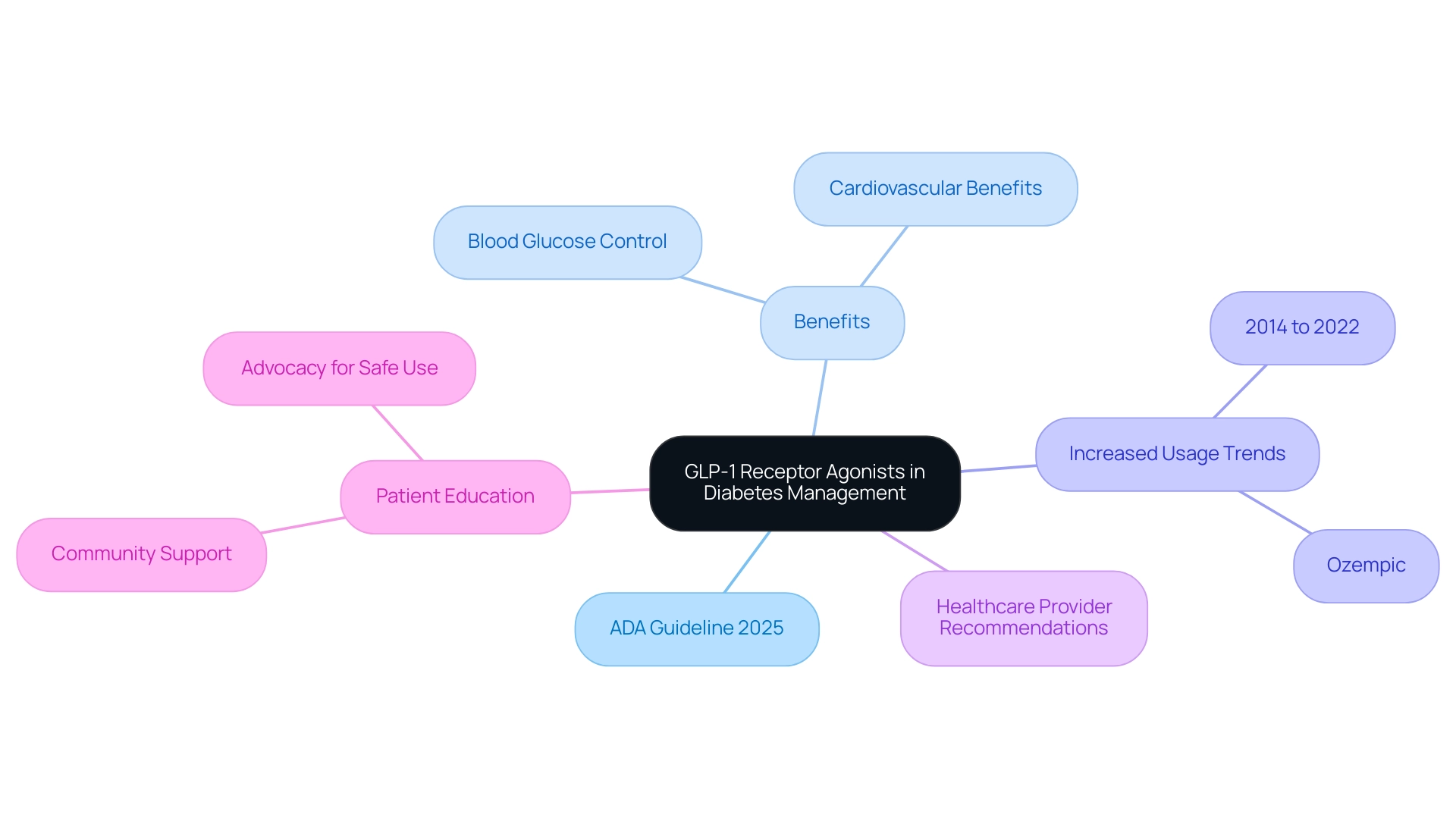
At T2DSolutions, we are committed to providing comprehensive resources for diabetes management. The ADA guideline 2025 highlights the important role of GLP-1 receptor agonists in managing diabetes, particularly for individuals with cardiovascular disease or those at increased risk. These medications not only help lower blood glucose levels but also offer significant cardiovascular benefits, making them a dual-purpose treatment option. We encourage healthcare providers to consider GLP-1 receptor agonists as a first-line therapy for suitable individuals, reflecting a strong body of evidence that supports their efficacy and safety.
Recent studies, including a retrospective cohort analysis from the University of California Health Data Warehouse, reveal a significant increase in the use of GLP-1 receptor agonists, especially Ozempic, among individuals with Type 2 Diabetes, cardiovascular disease, and obesity from 2014 to 2022. This trend indicates a lasting shift in treatment patterns, particularly for therapies associated with weight loss, further validating the cardiovascular advantages of these medications.
Moreover, we urge healthcare professionals to advocate for the safe use and dispensing of compounded Semaglutide to reduce risks related to severe adverse events and unnecessary hospitalizations. Specialists emphasize the importance of informing individuals about the benefits and correct usage of GLP-1 receptor agonists to optimize health management and improve overall health outcomes. As Pierce Logan, a Graduate Assistant at the Indiana University Center for Bioethics, asserts, "Doctors must be conscious of these facts, and patients should be educated."
The ADA guideline 2025 reflects a growing consensus on the cardiovascular benefits of GLP-1 receptor agonists, with statistics showing that these medications can significantly lower the risk of major cardiovascular events. Importantly, case studies have indicated no serious complications, such as pancreatitis or hypoglycemia, related to GLP-1 analog overdoses, further reinforcing their safety profile. This dual benefit not only aids in blood sugar control but also enhances cardiovascular health, making GLP-1 receptor agonists a vital component of modern care strategies for those managing high blood sugar.
At T2DSolutions, we aim to support you on this journey by providing a platform for community and collaboration. Managing diabetes is a collective effort, and we believe that shared knowledge and support can lead to improved health outcomes for everyone involved. Remember, you're not alone in this journey; we are here to support you every step of the way.
New Guidance for Diabetes Care in Older Adults
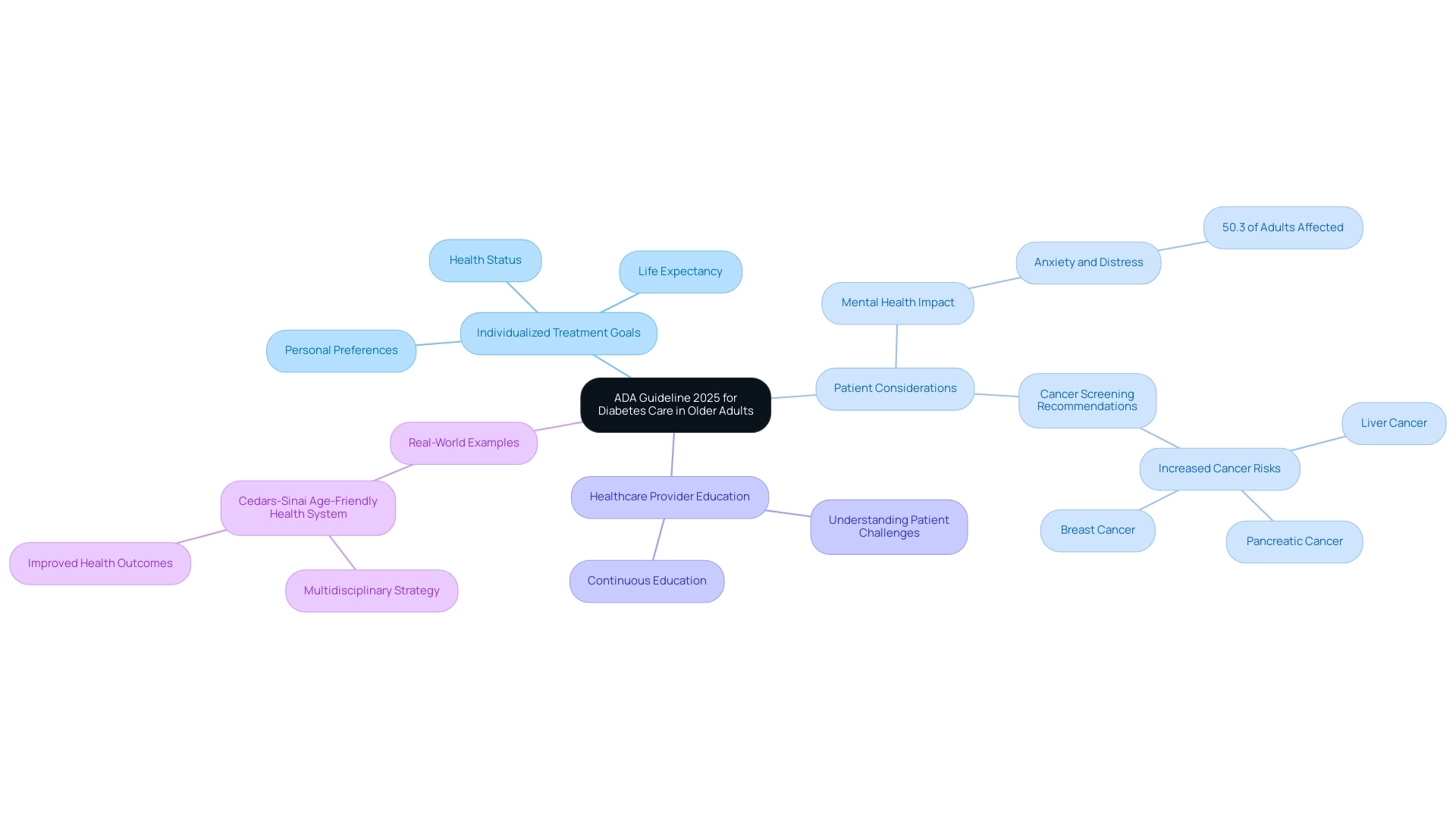
The ADA Guideline 2025 introduces significant advancements in managing blood sugar issues among older adults, emphasizing the necessity of individualized treatment goals. These goals are thoughtfully tailored to each person's overall health status, life expectancy, and personal preferences, ensuring that care is both relevant and effective. Regular evaluations across medical, psychological, and functional areas are essential, as they enable a thorough understanding of each patient's distinct requirements.
Healthcare providers are encouraged to carefully weigh the potential risks and benefits of medications for older patients. This cautious approach is particularly important, especially considering that nearly 50.3% of adults with diabetes also experience anxiety or severe diabetes distress, which can complicate treatment plans. By prioritizing personalized support, the ADA Guideline 2025 aims to improve the quality of life for older adults living with diabetes.
Real-world examples illustrate the effectiveness of these individualized treatment goals. For instance, Cedars-Sinai has implemented an Age-Friendly Health System that employs a multidisciplinary strategy to enhance services for older patients. Their collaborative efforts have led to notable improvements in health outcomes, showcasing the benefits of a tailored approach to managing blood sugar.
This system beautifully illustrates how personalized treatment objectives can be successfully incorporated into practice. Furthermore, the ADA Guideline 2025 highlights the significance of continuous education and assistance for healthcare providers, ensuring they are prepared to handle the intricacies of care in older adults. By fostering a deeper understanding of the unique challenges faced by this population, the ADA Guideline 2025 aims to empower both patients and providers in their shared journey toward better health outcomes.
Additionally, it's crucial for individuals with diabetes to undergo recommended cancer screenings, as this condition is associated with an increased risk of several cancers, including liver, pancreas, and breast cancer. Remember, you're not alone in this journey—support is available to help you navigate these challenges.
Importance of Emotional Health Screening in Diabetes Care
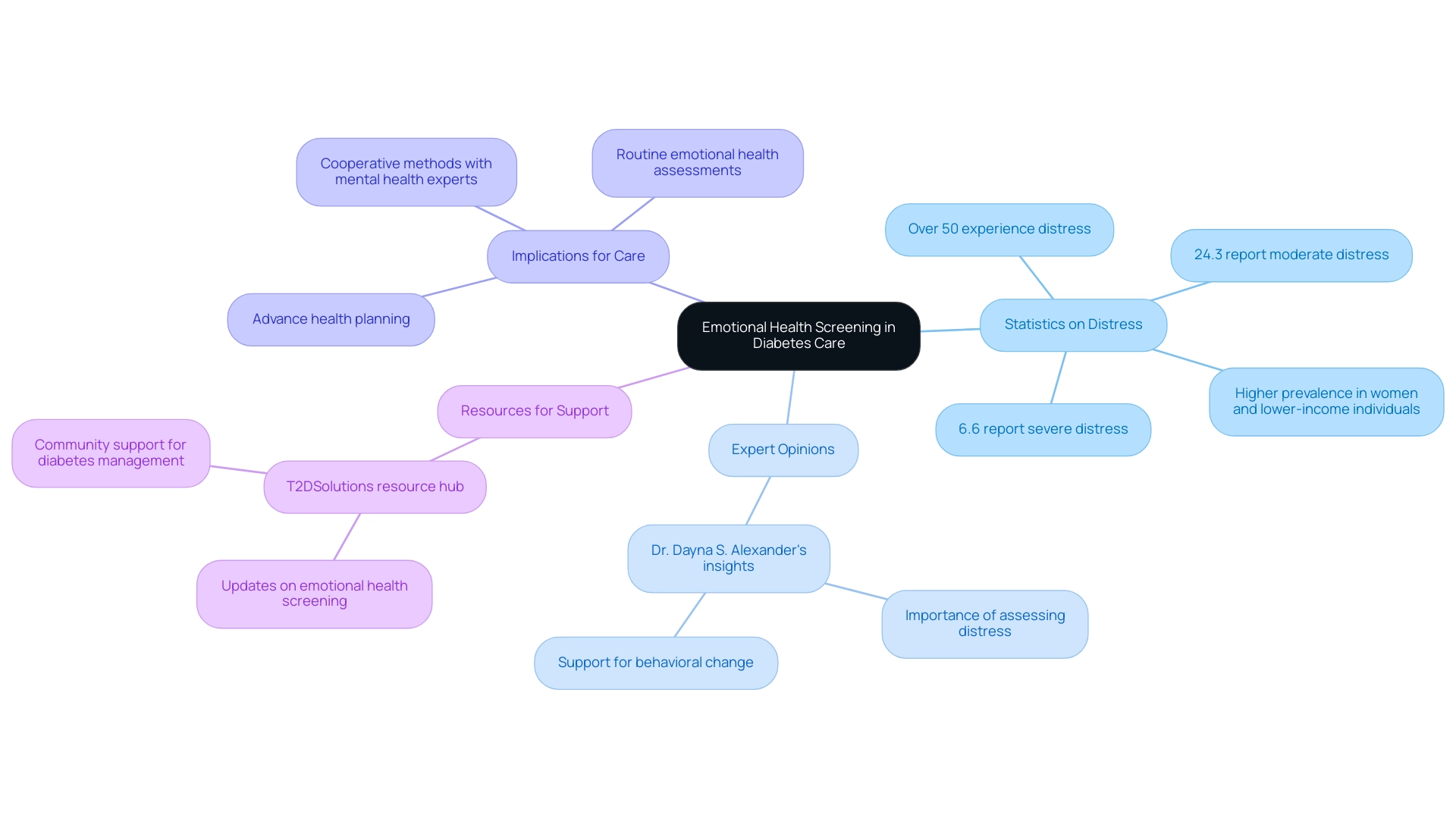
The ADA guideline 2025 emphasizes the crucial role of emotional health screening in managing your condition. It recognizes that individuals facing this illness often experience an increased risk of mental health issues, such as depression and anxiety. Routine evaluations are suggested to detect these conditions early, as they can significantly impact the management of blood sugar. Research shows that over half of US adults with this condition experience related distress, with 24.3% reporting moderate distress and 6.6% severe distress, particularly among those aged 18 to 64, women, and individuals with lower incomes.
This highlights the importance of incorporating emotional health assessments into routine management practices. You're not alone in this journey; understanding your emotional health can lead to better overall care.
Furthermore, advance health planning is essential for individuals with blood sugar issues. It enables you to specify your values and preferences for treatment, especially as you approach end-of-life choices. Addressing emotional well-being is crucial for effective management of your condition, as mental health directly affects treatment adherence and lifestyle choices. The ADA guideline 2025 promotes a cooperative method, encouraging healthcare teams to include mental health experts in the management of chronic conditions.
As Dr. Dayna S. Alexander states, "Thus, prior findings demonstrate the importance of assessing distress among individuals living with this condition to support behavioral change by implementing multilevel, culturally tailored interventions." This expert opinion emphasizes that evaluating distress related to blood sugar management can support behavioral changes, ultimately leading to improved health outcomes.
Real-world examples demonstrate the effect of mental health on blood sugar management. For instance, a cross-sectional study utilizing data from the 2021 National Health Interview Survey revealed the emotional and psychological difficulties faced by individuals managing their condition. By prioritizing emotional health screening, healthcare providers can empower you to navigate your condition journey more effectively, fostering resilience and enhancing your overall quality of life.
As T2DSolutions launches as a new resource hub for Type 2 and Type 3 blood sugar education and community support, it will provide essential resources and assistance related to emotional health screening in condition oversight. We invite you to subscribe for updates on how T2D Solutions will assist you in managing your condition effectively, ensuring that emotional well-being is a key component of your care.
Updated Nutrition Guidance for Diabetes Management
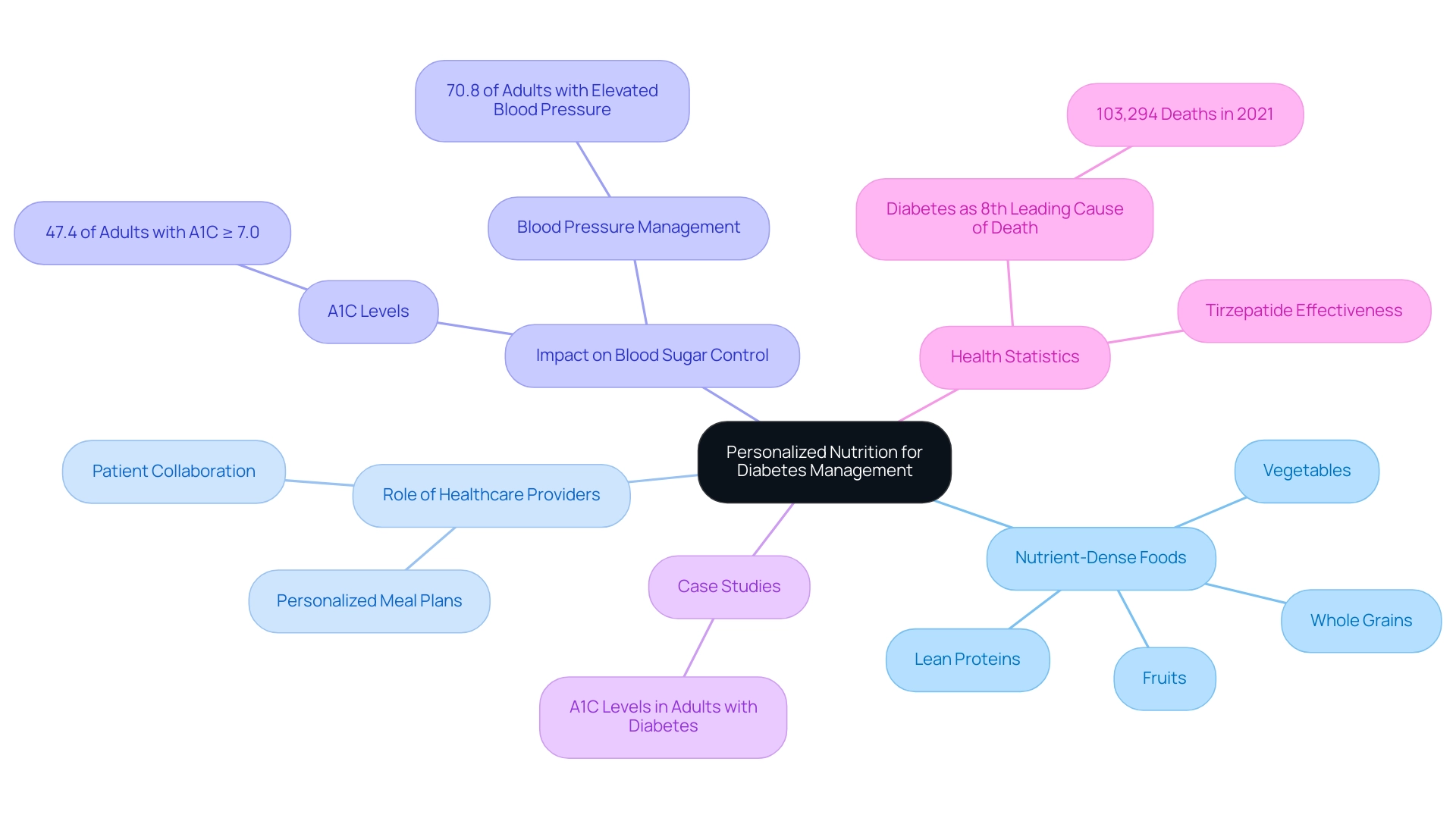
The ADA guideline 2025 introduces important revisions to nutrition advice, emphasizing the significance of personalized dietary plans for effective health control. These recommendations advocate for the inclusion of nutrient-dense foods such as whole grains, fruits, vegetables, and lean proteins, while encouraging a reduction in processed foods and added sugars. This tailored approach invites healthcare providers to work alongside patients in creating personalized meal plans that align with their unique preferences and lifestyles, fostering sustainable dietary changes.
It's understandable to feel overwhelmed by dietary choices, especially when managing health conditions. Studies highlight the crucial role of personalized nutrition in controlling blood sugar levels. For instance, data reveals that 47.4% of adults with diabetes have an A1C value of 7.0% or higher, indicating a pressing need for improved dietary strategies. The case study titled "A1C Levels in Adults with Diabetes" illustrates significant variations across age groups, underscoring the challenges in achieving optimal management of this condition.
By focusing on personalized nutrition, the guidelines aim to enhance blood glucose control and improve overall health outcomes.
Moreover, the importance of personalized dietary plans is underscored by the fact that 70.8% of U.S. adults with diagnosed conditions experience elevated blood pressure levels, which can be effectively managed through proper nutrition. The ADA guideline 2025 not only addresses these health concerns but also emphasizes the need to adapt dietary recommendations to meet the specific needs of each patient. According to the American Diabetes Association Professional Practice Committee, "The handling of this condition in elderly individuals at the end of life requires a person-centered approach that emphasizes comfort, symptom control, quality of life, and the maintenance of dignity."
Real-world examples demonstrate the effectiveness of individualized dietary plans. Many patients who have successfully implemented tailored meal strategies report improved glycemic control and a better quality of life. This comprehensive approach to nutrition not only aids in regulating blood glucose levels but also enhances the overall wellness of individuals living with diabetes, reinforcing the idea that effective management of the illness is a personalized journey.
With diabetes ranking as the eighth leading cause of mortality in the United States, the need for effective nutritional approaches in managing it is more critical than ever. Remember, you're not alone in this journey; we are here to support you every step of the way.
Implications of the 2025 ADA Guidelines for Patients and Providers
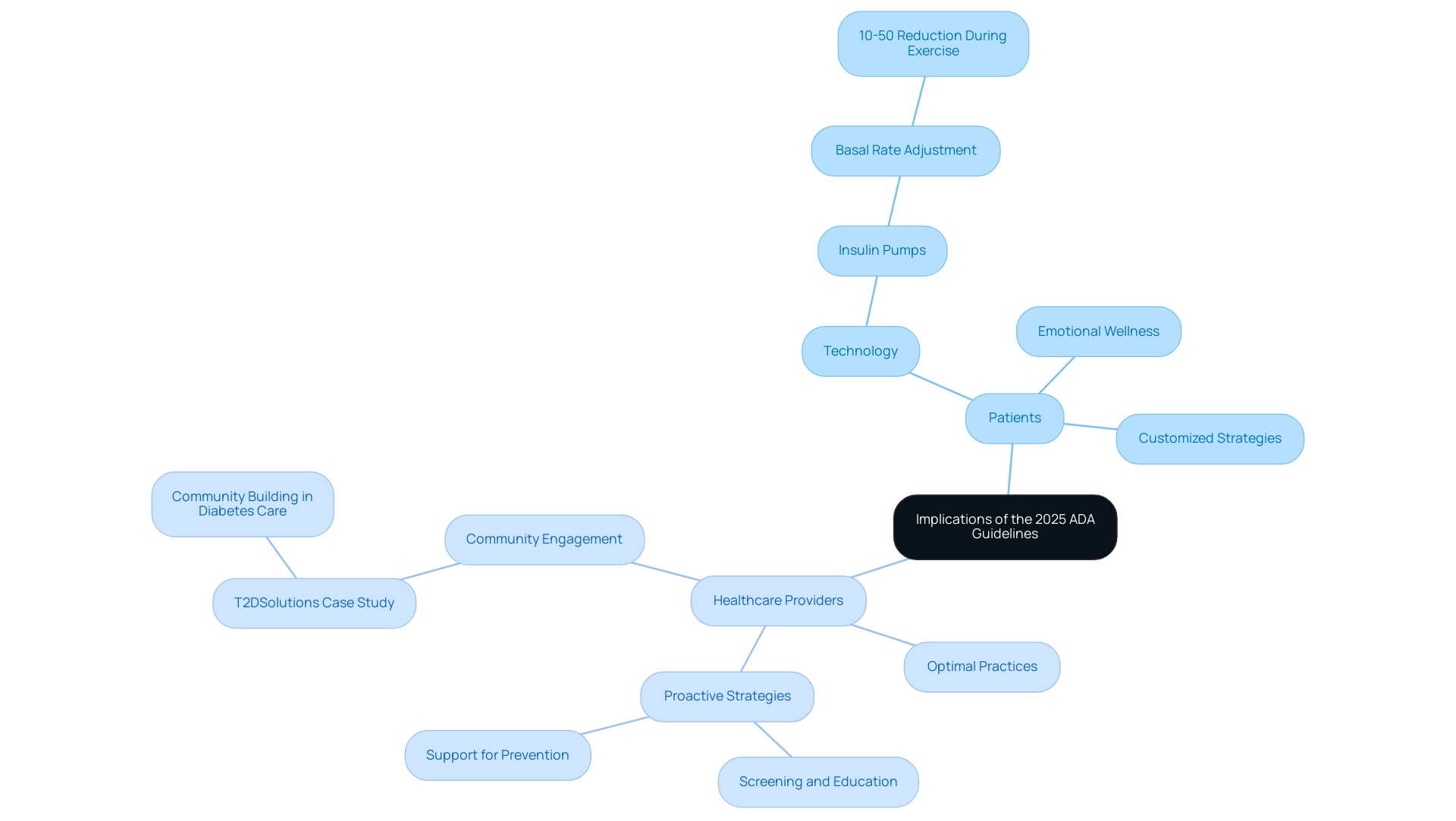
The ADA Guideline 2025 presents crucial implications for individuals managing blood sugar issues and their healthcare providers. For patients, these updates create a clearer structure for effective health oversight, emphasizing the importance of technology, emotional wellness, and tailored approaches. Significantly, the incorporation of advanced devices, such as insulin pumps, allows young individuals to adjust basal rates by approximately 10–50% during physical activity, underscoring the opportunity for customized strategies.
Healthcare professionals also benefit from these guidelines, as they serve as a comprehensive resource for implementing optimal practices in health treatment. By adhering to the latest recommendations, providers can enhance their treatment strategies. This is especially important given the notable rise in medical expenses related to diabetes management, which increased from $10,179 in 2012 to $12,022 in 2022. This financial burden highlights the urgent need for proactive efforts in screening, education, and support for prevention and management of the condition.
As Erin Byrne, MPH, observes, 'The ADA Guideline 2025 highlights the significance of a proactive strategy in diabetes management, ensuring that both individuals and providers are prepared to handle the intricacies of this condition.' It’s understandable to feel overwhelmed, but these guidelines advocate for a collaborative approach, promoting open communication between patients and providers. This partnership is vital for ensuring that care is customized to meet individual needs, ultimately leading to improved health outcomes.
Real-world examples demonstrate that adherence to the ADA Guideline 2025 can lead to significant health improvements. This reinforces the importance of these standards in fostering resilience and hope among those managing the condition. T2DSolutions exemplifies this through its focus on community engagement, as highlighted in the case study 'Community Building in Diabetes Care.' This illustrates how shared experiences can enhance the collective journey of health oversight, making the implications of the ADA Guideline 2025 even more impactful. As T2DSolutions continues to develop as a resource hub, it will provide valuable information and support related to the ADA Guideline 2025, helping newly diagnosed patients navigate their diabetes management effectively. Remember, you're not alone in this journey, and we are here to support you every step of the way.
Conclusion
The 2025 ADA Guidelines represent a significant step forward in diabetes care, focusing on personalized strategies, emotional well-being, and innovative technologies. By incorporating Continuous Glucose Monitoring (CGM) for Type 2 Diabetes patients, these guidelines empower individuals to make informed decisions and achieve better glycemic control, while also reducing the risk of hypoglycemic events. Additionally, the expanded role of GLP-1 receptor agonists underscores the importance of medications that support both diabetes management and cardiovascular health.
For older adults, the guidelines advocate for individualized treatment goals that are sensitive to each patient's unique circumstances. This approach not only enhances the quality of care but also fosters a deeper understanding of the patient's needs. Recognizing emotional health as a vital component of diabetes management encourages healthcare providers to assess and support their patients' mental well-being, which can lead to improved health outcomes.
Updated nutrition guidance emphasizes personalized dietary plans centered around nutrient-dense foods, which play a crucial role in managing blood glucose levels and addressing related health issues, such as hypertension.
Together, these guidelines provide a comprehensive framework for healthcare providers, equipping them with best practices to enhance patient outcomes. By encouraging open communication and collaboration between patients and providers, the guidelines ensure that care is tailored to individual needs.
In summary, the 2025 ADA Guidelines offer invaluable support for both patients and healthcare professionals. They create an opportunity to improve health outcomes and enhance the quality of life for millions living with diabetes. Remember, you're not alone in this journey; we are here to support you every step of the way.



