Overview
Managing diabetes can feel overwhelming, but understanding your metrics can empower you on this journey. The article compares A1C and average glucose levels, two essential tools for monitoring your blood sugar control. Each serves a distinct purpose: A1C reflects long-term glucose regulation, while average glucose offers insights into daily fluctuations.
It's understandable to feel confused about these terms, but grasping their roles is crucial. By recognizing how A1C provides a snapshot of your overall control and how average glucose reveals day-to-day patterns, you can work more effectively with your healthcare team to develop treatment strategies tailored to your needs.
You're not alone in this journey. Many individuals find that understanding these metrics leads to improved health outcomes and a greater sense of control. We are here to support you every step of the way, encouraging you to seek resources and ask questions that will help you navigate your diabetes management with confidence.
Introduction
In the realm of diabetes management, it’s essential to understand the nuances of A1C and average glucose levels. These two metrics provide distinct yet complementary insights into blood sugar control, each playing a pivotal role in shaping effective treatment strategies. A1C acts as a long-term indicator, reflecting your average blood glucose over the past two to three months. On the other hand, average glucose offers a snapshot of daily fluctuations, which is crucial for real-time management.
As diabetes care evolves, integrating these measurements, along with advancements in technology and personalized approaches, is transforming how individuals navigate their health journeys. This article will explore the significance of A1C and average glucose, delving into their definitions, measurement methods, and the implications for effective diabetes management. Remember, you're not alone in this journey; we are here to support you every step of the way.
Understanding A1C and Average Glucose: Definitions and Importance
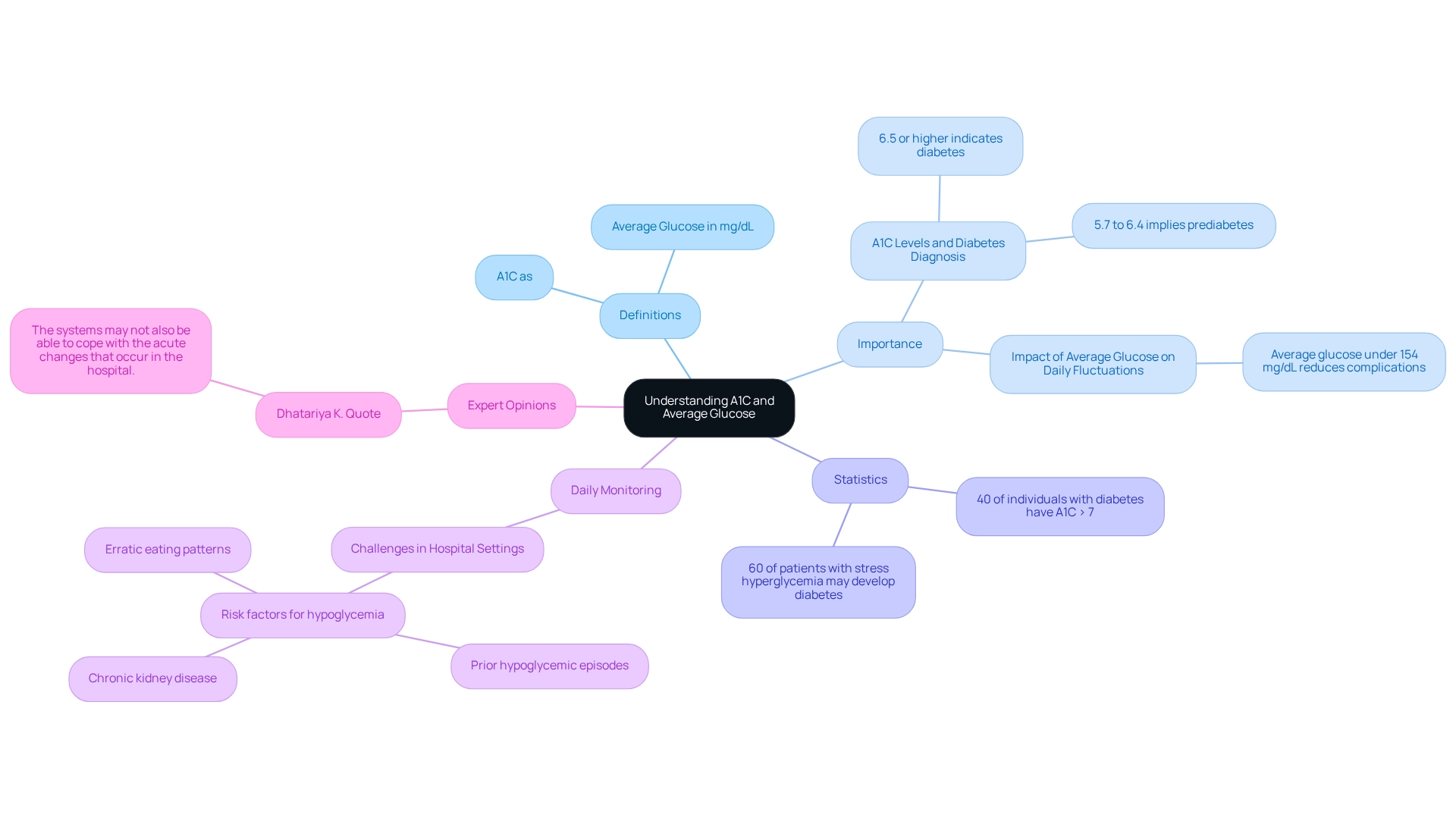
A1C, or glycated hemoglobin, is an essential blood test that helps compare A1C versus average glucose levels over the prior two to three months. Expressed as a percentage, it indicates the proportion of hemoglobin molecules that have sugar attached to them, serving as a long-term marker of sugar regulation. In contrast, average blood sugar represents the estimated average blood sugar levels during the same timeframe, typically measured in mg/dL.
Both metrics—A1C and average glucose—are vital for effectively managing blood sugar levels, offering complementary insights into glucose control. Understanding A1C is crucial for diagnosing diabetes and assessing treatment effectiveness. For instance, an A1C level of 6.5% or higher indicates diabetes, while levels between 5.7% and 6.4% imply prediabetes. Recent statistics reveal that approximately 40% of individuals with diabetes have an A1C level above the recommended target of 7%, highlighting the need for improved management strategies.
On the other hand, average blood sugar provides a more immediate perspective on daily fluctuations. This metric can be especially beneficial for patients tracking their sugar levels throughout the day, as it reflects the impact of meals, physical activity, and medication adherence. For example, a study found that patients who maintained an average glucose level under 154 mg/dL encountered fewer complications associated with their condition, underscoring the importance of daily monitoring.
As T2DSolutions launches as a new resource hub for Type 2 and Type 3 blood sugar management education, understanding these metrics becomes even more crucial for newly diagnosed patients. Case studies further illustrate the importance of these metrics in controlling blood sugar levels. One study on the pathophysiology of hyperglycemia during illness revealed that non-diabetic individuals could experience heightened sugar levels due to stress and hormonal responses, emphasizing the need for effective intervention strategies in hospitalized patients.
This research suggests that as many as 60% of patients with stress hyperglycemia may develop confirmed metabolic disorder within 6 to 12 months after discharge, making it vital to track both A1C and average glucose levels during and after hospital stays. Furthermore, typical risk factors for experiencing hypoglycemia in hospitals include previous hypoglycemic occurrences, chronic kidney disease, and irregular eating habits, which highlight the challenges of controlling blood sugar levels in various environments.
Expert opinions also stress the necessity of understanding these metrics. Professionals in the field emphasize that while A1C provides a long-term perspective on glucose regulation, examining A1C versus average glucose offers insights into daily oversight, making both crucial for comprehensive care. Dhatariya K. notes that "the systems may not also be able to cope with the acute changes that occur in the hospital," underlining the difficulties faced in overseeing care for patients with diabetes during hospitalization.
By incorporating these measurements into their management strategies, individuals can navigate their condition journey more effectively, leading to enhanced health outcomes. You're not alone in this journey; we are here to support you every step of the way.
How A1C Levels Are Measured and Interpreted
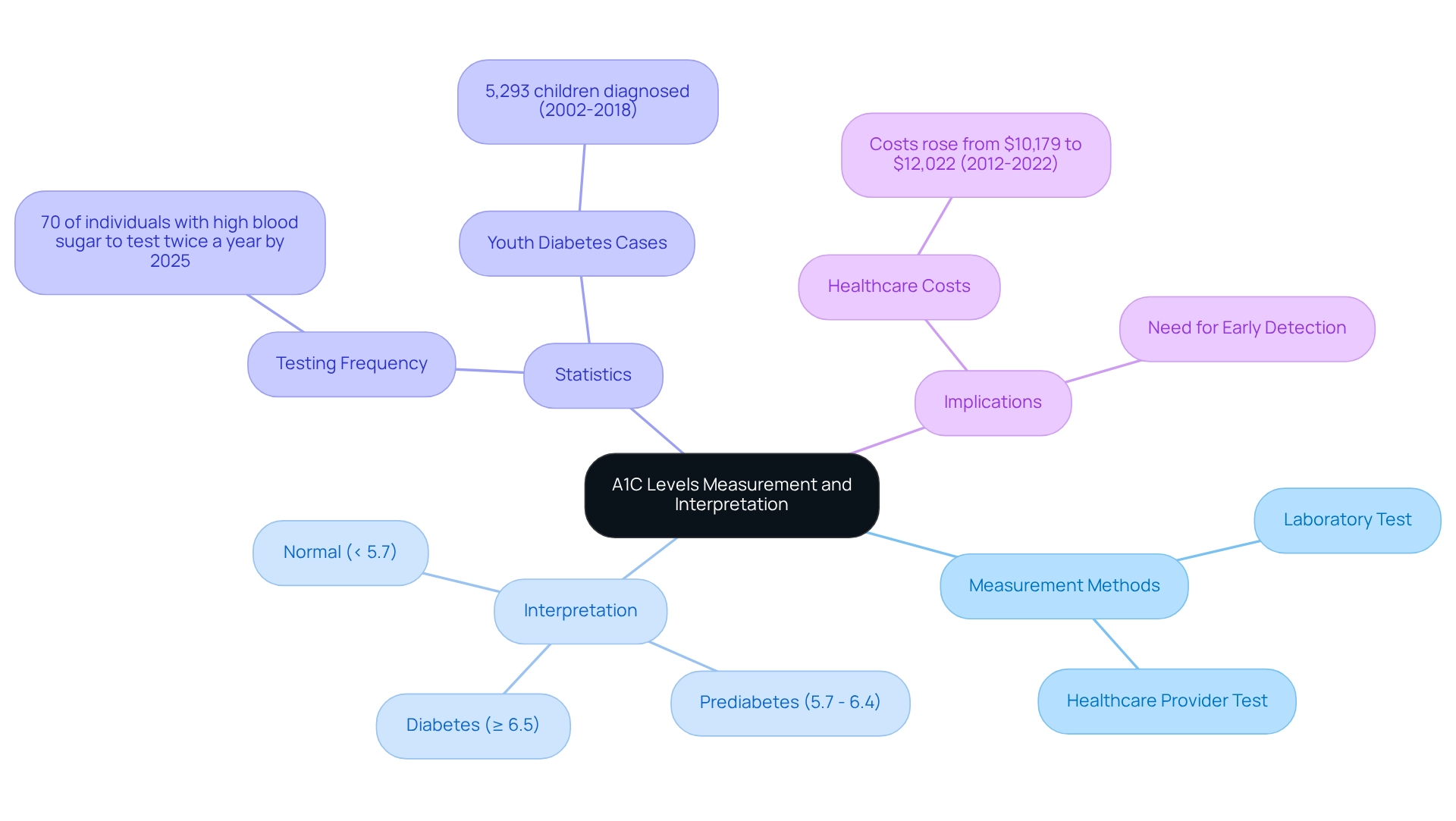
A1C levels are determined through a straightforward blood test, which can be conducted either in a laboratory or at a healthcare provider's office. This test measures the percentage of glycated hemoglobin, allowing you to compare A1C vs. average glucose levels over the past two to three months. Results are typically expressed as a percentage, with a normal A1C level being below 5.7%.
If your levels fall between 5.7% and 6.4%, it suggests prediabetes, while an A1C of 6.5% or above confirms a diagnosis of the condition. Understanding these thresholds is essential for you, as it helps gauge your risk and recognize the necessity for lifestyle modifications or medical interventions.
Recent statistics highlight the importance of regular A1C testing among individuals with blood sugar issues. By 2025, it's estimated that roughly 70% of individuals with high blood sugar will undergo A1C testing at least twice a year, underscoring the test's role in ongoing healthcare. Alarmingly, case studies from the SEARCH for Diabetes in Youth study reveal that 5,293 children and adolescents aged 10 to 19 years were diagnosed with type 2 conditions from 2002 to 2018. This emphasizes the urgent need for early detection and intervention through A1C monitoring.
This trend is further compounded by the escalating healthcare expenses linked to the condition, which rose from $10,179 to $12,022 per individual between 2012 and 2022, emphasizing the financial consequences of insufficient care.
At T2DSolutions, we acknowledge the significance of A1C testing as a component of a thorough health care plan. Our mission is to provide newly diagnosed patients with the resources and support they need to understand their A1C results and make informed decisions about their health. Healthcare professionals highlight the significance of interpreting A1C results when considering A1C vs. average glucose within the framework of a comprehensive management plan for the condition.
For instance, Eyth E. observes that "Hemoglobin A1c is an important tool in managing metabolic disorders and other glycemic control issues, but it operates most effectively within a collaborative healthcare team setting to achieve optimal results." This emphasizes the cooperative approach required for effective care, where A1C testing acts as a vital element in evaluating and modifying treatment strategies.
You're not alone in this journey. T2DSolutions is here to support you, offering educational materials and community resources to help you manage your diabetes effectively.
Calculating Average Glucose: Methods and Significance
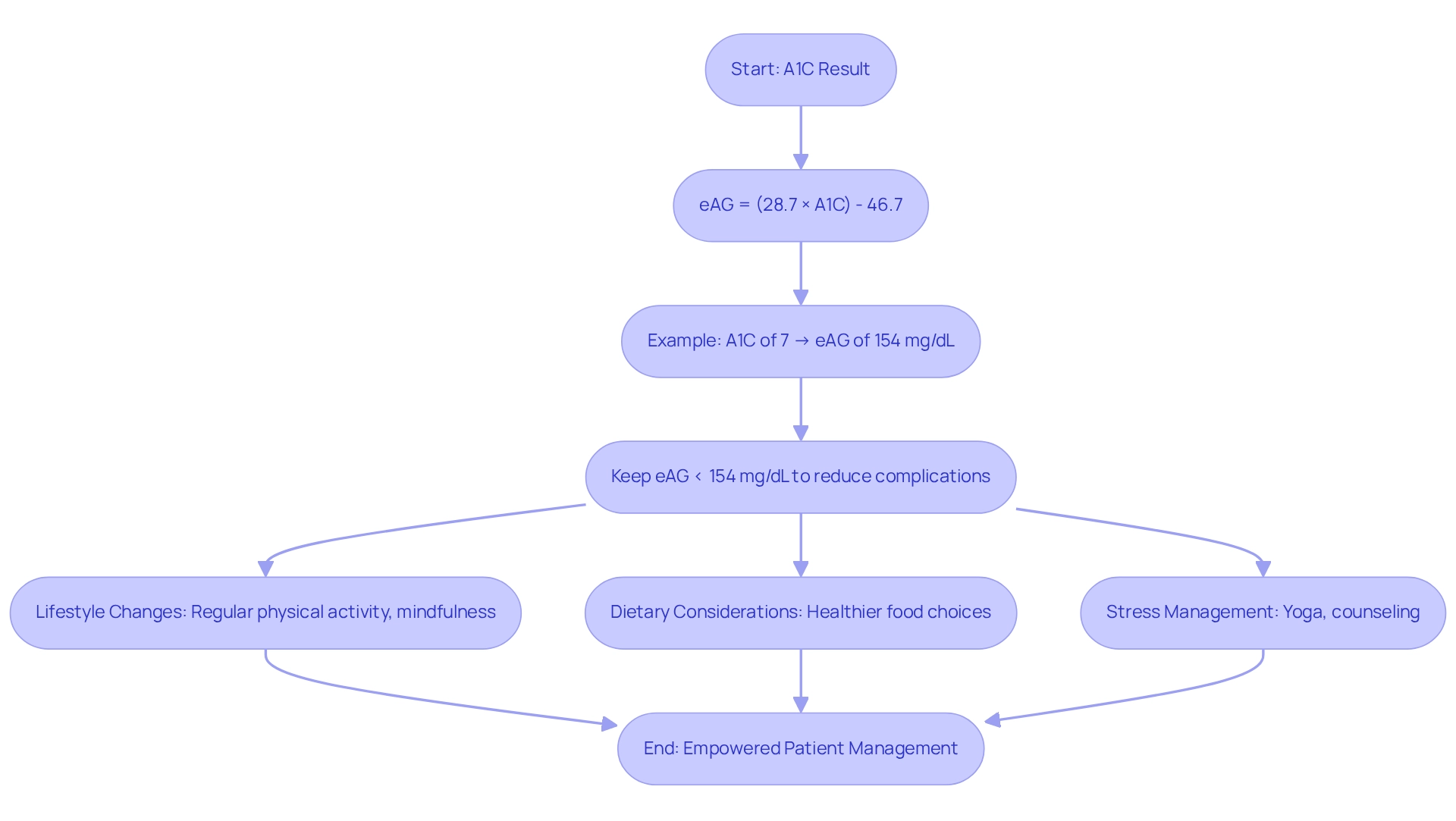
Average sugar levels can be estimated from A1C results using the formula:
eAG (estimated average sugar) = (28.7 × A1C) - 46.7.
This calculation converts the percentage of A1C into a more recognizable blood sugar measurement, typically expressed in mg/dL. For instance, an A1C of 7% relates to an average sugar level of roughly 154 mg/dL, which is the goal for many individuals living with diabetes.
Grasping this conversion is essential for patients, as it connects laboratory results with daily sugar monitoring. This understanding enables more effective control of their condition, fostering a sense of empowerment.
The importance of average sugar levels in diabetes management cannot be overstated. Research indicates that maintaining an estimated average sugar level below 154 mg/dL can significantly reduce the risk of diabetes-related complications. This knowledge empowers patients to set realistic goals and monitor their progress more effectively.
The eAG calculator is particularly beneficial, helping healthcare providers report A1C results in familiar units for patients. This enhances their comprehension of these critical metrics, making the journey a bit easier.
Expert opinions highlight the importance of average glucose in providing a clearer picture of overall glycemic control. Julia Zakrzewski, a registered dietitian, emphasizes that "a registered dietitian is a nutrition expert and licensed healthcare professional," underscoring the value of professional guidance in interpreting these results.
Furthermore, dietary considerations play a vital role in managing blood sugar levels. For instance, a recent article by Sarah Bullard, MS, RD, titled '9 Best Coffee Creamers For Diabetes,' discusses healthier coffee creamer options that do not elevate blood sugar levels. This illustrates the significance of mindful dietary choices in controlling the condition.
As T2DSolutions introduces itself as a fresh resource center for health education and community support, it will offer valuable articles, case studies, and expert insights to assist patients in comprehending and managing their A1C and average blood sugar levels effectively. Case studies demonstrate how patients have successfully employed average blood sugar calculations to improve their condition control. For example, individuals who actively engage in lifestyle changes—like regular physical activity, mindfulness practices, and stress control techniques—often report enhanced average blood sugar levels.
Chronic stress, which can negatively impact metabolic functions, including blood sugar regulation, highlights the necessity for comprehensive strategies in managing this condition. Engaging in activities like yoga and seeking professional counseling can significantly aid in managing stress and improving overall health outcomes.
In summary, understanding A1C vs average glucose is a vital aspect of diabetes management. By learning how to calculate and interpret these values, patients can take proactive steps toward achieving better health and quality of life. Remember, you're not alone in this journey. To stay updated on new content and resources from T2D Solutions, consider subscribing for email notifications.
The Relationship Between A1C and Average Glucose: What You Need to Know
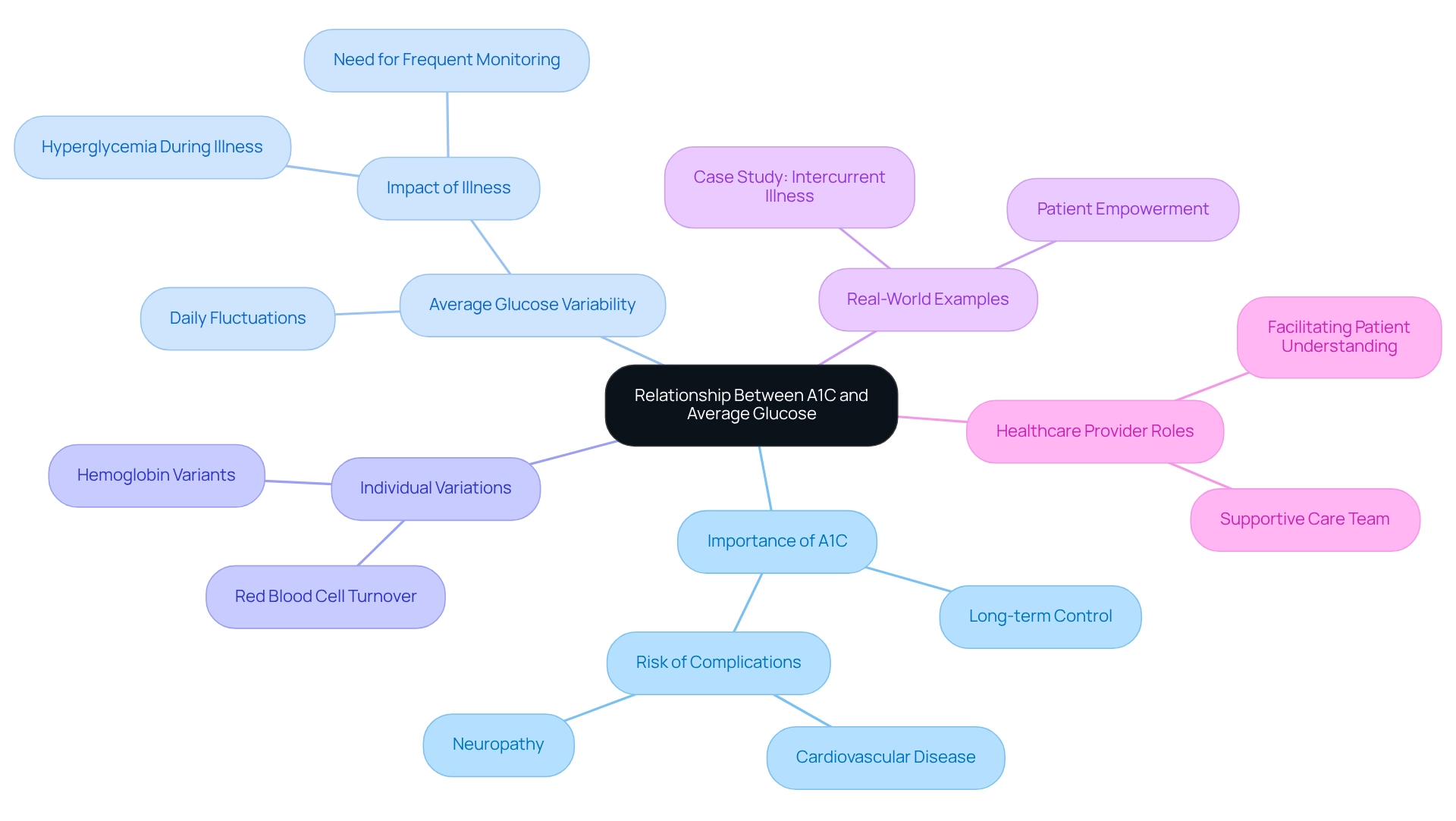
Understanding the connection between A1C and average glucose is crucial for anyone managing diabetes. Many studies have shown a strong relationship between these two metrics, and it's important to recognize how they reflect your blood sugar management. A1C serves as a valuable indicator of long-term control, showing average blood sugar levels over the past two to three months. In contrast, average glucose captures daily fluctuations. Generally, a higher A1C indicates poorer blood sugar control, which can increase the risk of complications like cardiovascular disease and neuropathy.
However, it’s essential to remember that individual variations can complicate this relationship. For some, discrepancies between A1C and average glucose levels may arise due to factors like hemoglobin variants or changes in red blood cell turnover. This highlights the need for personalized strategies in blood sugar management that consider these unique differences.
Real-world examples illustrate the significance of this connection. During illnesses—such as infections or surgeries—many patients experience hyperglycemia, which requires more frequent monitoring and possible adjustments to treatment. In these moments, having a supportive care team is vital to effectively manage complications and maintain optimal glycemic control.
Research indicates that understanding the relationship between A1C and average glucose can empower patients to take a more active role in their health. By expressing A1C in average sugar units, healthcare providers can facilitate clearer discussions, enhancing your understanding and involvement in your care. This is especially important for those newly diagnosed, as interpreting A1C values can be challenging.
Additionally, the Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications (DCCT/EDIC) Research Group found that effective treatment can have long-term benefits for cognitive function, underscoring the importance of strong oversight strategies.
There is ongoing discussion about whether continuous glucose monitoring (CGM) is superior to glucometer self-monitoring for improving glycemic control. Understanding these tools can empower newly diagnosed patients in their management journey, making it easier to navigate your health.
In summary, grasping the relationship between A1C and average glucose is essential for tailoring diabetes management strategies to fit your individual needs. By doing so, you can work toward achieving better health outcomes. Remember, you're not alone in this journey; support is available to help you every step of the way.
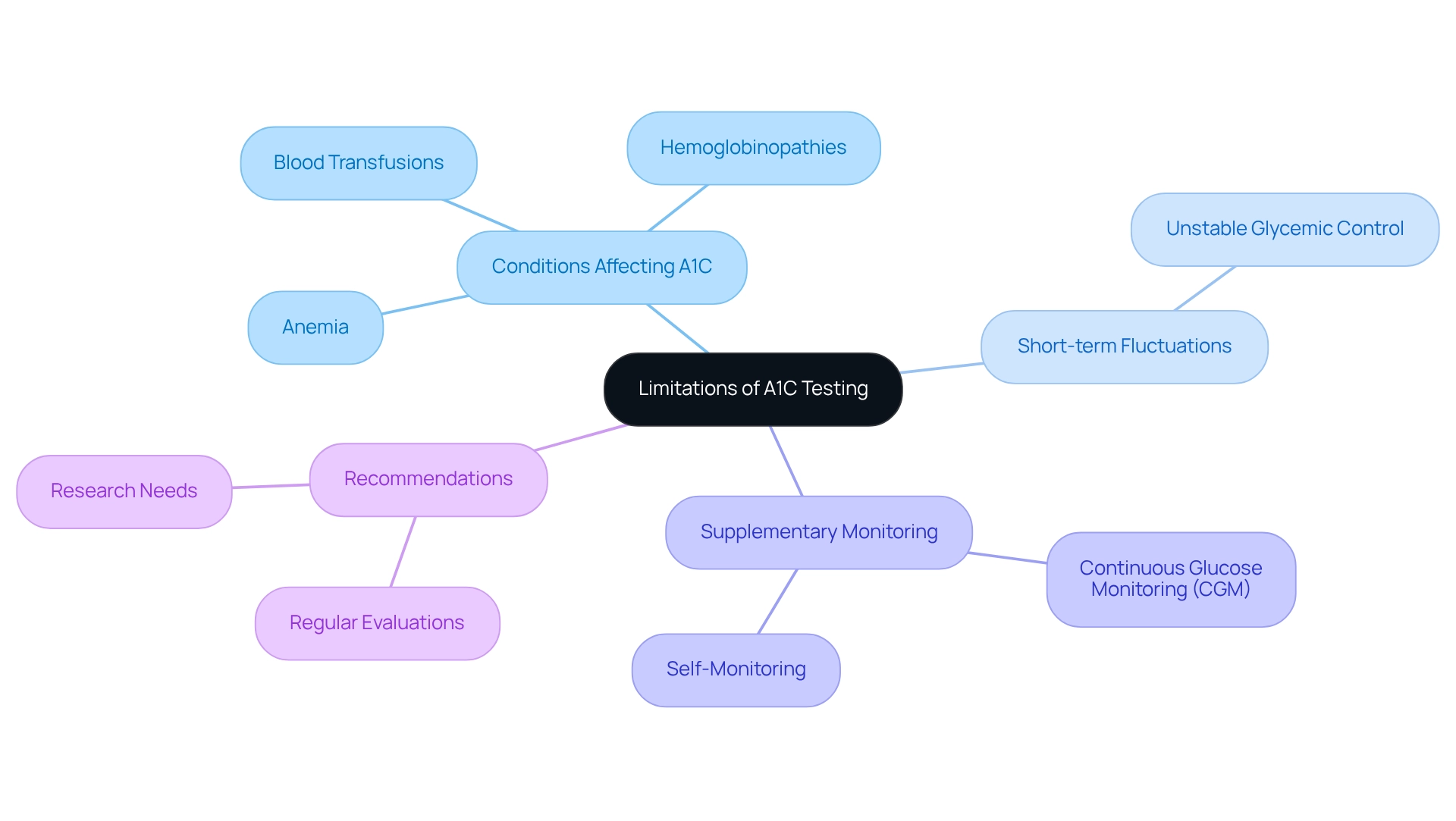
Limitations of A1C Testing: When It May Not Be Reliable
A1C testing is an essential tool for evaluating long-term sugar control, especially when comparing A1C to average glucose levels. However, it’s important to recognize its limitations. Conditions such as anemia and hemoglobinopathies can lead to misleading A1C results. Additionally, recent blood transfusions may artificially elevate or lower these values, which can be concerning.
Moreover, A1C testing may not capture short-term fluctuations in blood sugar levels, particularly in patients undergoing rapid changes. This is especially critical for individuals with unstable glycemic control, as it may not accurately reflect their current health status in the context of A1C versus average glucose.
To better navigate these challenges, healthcare providers often recommend supplementary monitoring techniques. Continuous glucose monitoring (CGM) systems and frequent self-monitoring of blood glucose can provide a more nuanced understanding of a patient’s glycemic control. For instance, consider a case study involving a 16-year-old obese African-American male diagnosed with metabolic syndrome. His condition progressed rapidly from pre-diabetes to complicated type 2 diabetes within just 7.5 weeks, highlighting the need for more proactive monitoring and intervention strategies.
As T2DSolutions emerges as a new resource hub for diabetes education and community support, it aims to offer valuable information and tools to help patients understand their A1C results and overall diabetes management. Experts emphasize the importance of regularly assessing self-monitored blood sugar readings to ensure they align with A1C results. As Stewart B. Harris wisely notes, "Periodic evaluation of self-monitored blood glucose readings is important to ensure concordance with HbA results."
This comprehensive approach not only enhances the management of diabetes but also empowers patients to take an active role in their healthcare journey. Furthermore, a systematic review suggests that early pregnancy HbA1c levels of 5.9% (41 mmol/mol) or higher are ideal for identifying diabetes, providing a relevant benchmark for understanding A1C testing limitations. As we move forward, continuous research will be vital in improving screening techniques and enhancing the accuracy of blood sugar evaluations.
Additionally, further investigation is needed to assess the feasibility, effectiveness, and cost-effectiveness of screening for blood sugar issues in dental settings. This could provide deeper insights into the broader implications of health strategies, ensuring that we are all better equipped in our journeys toward health.
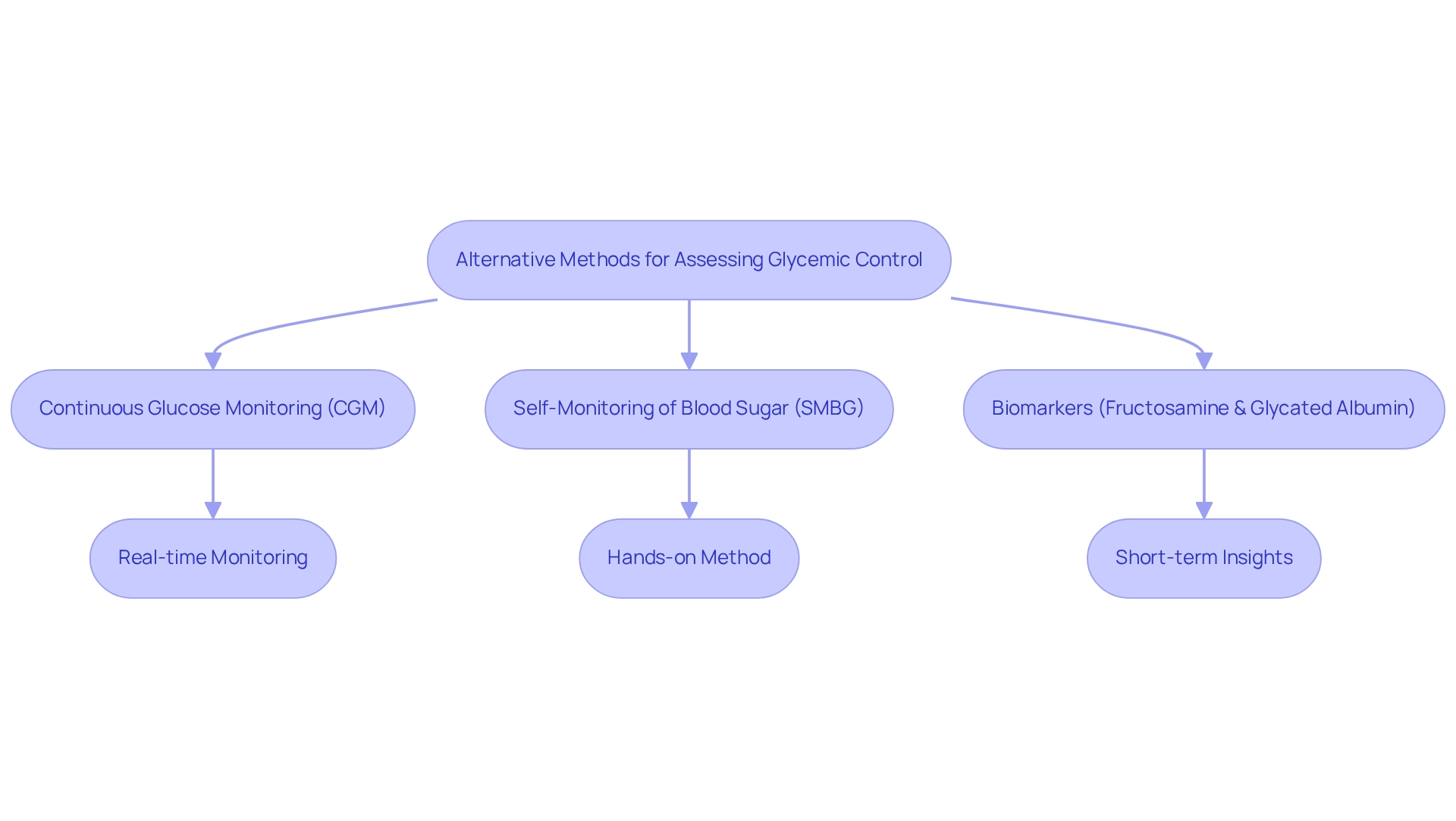
Alternative Methods for Assessing Glycemic Control
In addition to A1C testing, various alternative methods are available for assessing glycemic control, each offering unique advantages. Continuous glucose monitoring (CGM) stands out by providing real-time glucose readings, enabling patients to track their glucose levels throughout the day. This prompt feedback allows for timely modifications to management strategies, greatly improving blood sugar regulation.
Recent research has demonstrated that CGM technology can reduce hemoglobin A1c levels and enhance the overall quality of life for individuals with type 2 conditions, especially in primary care environments. As a result, there are increasing calls for revisions in insurance policies to improve access to this vital technology. Laura Wood, Senior Press Manager, remarked, "Millions of Americans are diagnosed with this condition each year, leading to a growing need for effective monitoring solutions."
At T2DSolutions, we understand the significance of these advancements in managing blood sugar. Our platform aims to serve as a comprehensive resource hub for individuals navigating their diabetes journey, providing education and support tailored to their needs. You're not alone in this journey, and we are here to support you every step of the way.
Alternative techniques for tracking sugar levels include self-monitoring of blood sugar (SMBG), which requires regular fingerstick tests. This conventional approach remains useful, particularly for patients who prefer a hands-on method of monitoring their sugar levels. Furthermore, biomarkers like fructosamine and glycated albumin can offer insights into shorter-term sugar management, making them beneficial for patients with conditions that may impact the comparison of A1C versus average glucose accuracy.
Statistics indicate that in 2025, the adoption of CGM technology is expected to rise, particularly among younger patients with private insurance and higher HbA1c values. Participants in recent studies reported an average of 5.8 prediagnostic CGM recordings alongside oral glucose tolerance tests (OGTT), highlighting the growing integration of CGM in managing blood sugar conditions. The case study titled "Impact of CGM on Diabetes Management" further supports this, exploring how CGM technology can aid in lowering hemoglobin A1c levels and enhancing the quality of life for individuals with type 2 conditions.
These alternative techniques not only improve the comprehension of glycemic control but also empower patients to take a proactive role in their health care. It's understandable to feel overwhelmed, but remember that there are resources and support systems available to help you navigate your path to better health.
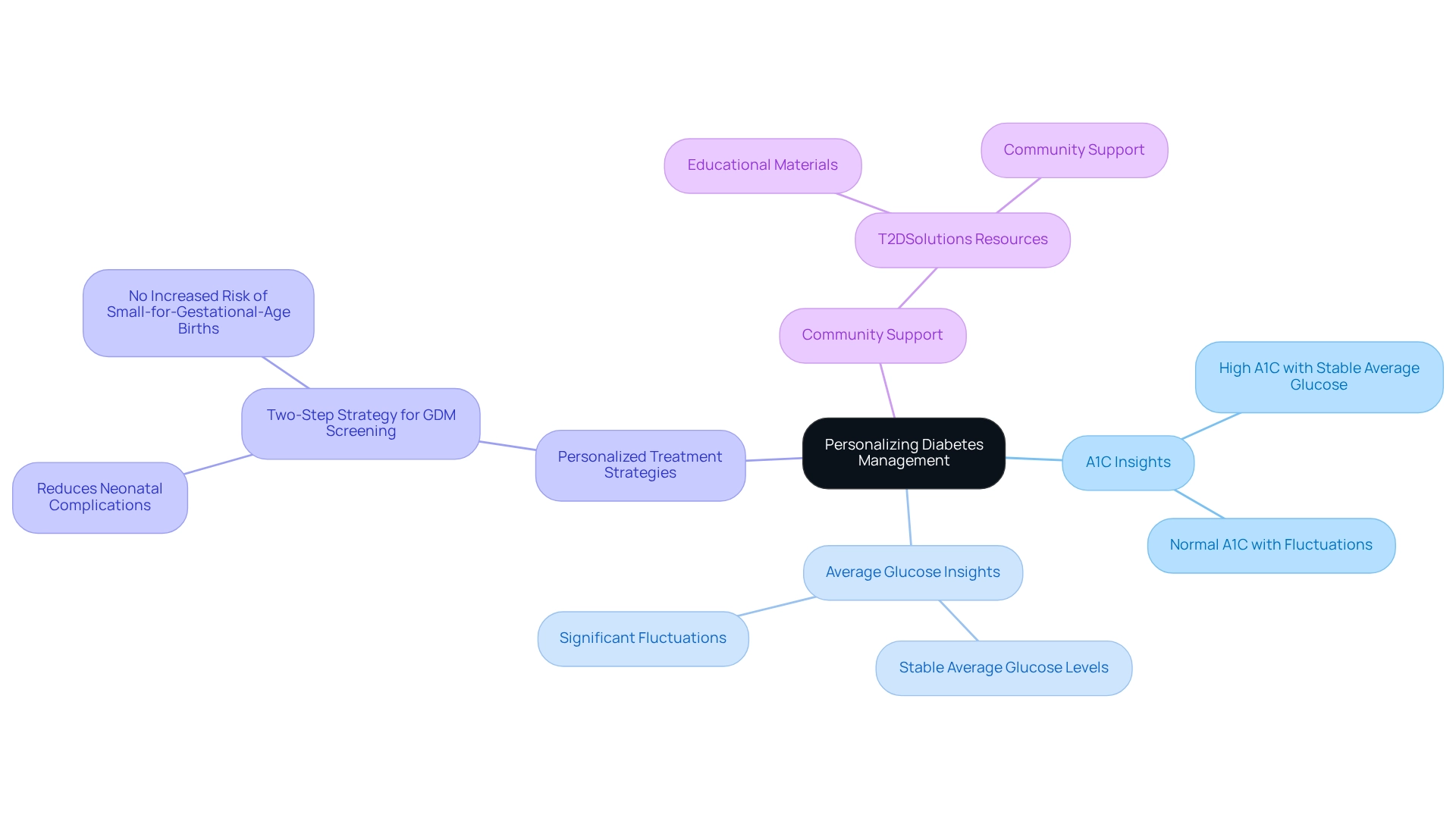
Personalizing Diabetes Management: Integrating A1C and Average Glucose Insights
Customizing care for blood sugar conditions requires a compassionate understanding of both A1C and average glucose. These metrics, while related, offer distinct insights into a patient's glycemic control. For example, a patient with a high A1C but stable average blood sugar levels may need a different approach than someone with a normal A1C but significant fluctuations in blood sugar.
This personalized approach not only fosters greater patient engagement but also leads to improved diabetes management outcomes. It's important to note that research shows 28% of the time, the glucose management indicator (GMI) and laboratory A1C differ by 0.5% or more. This highlights why analyzing A1C and average glucose is vital for healthcare providers when creating treatment plans. By tailoring interventions to individual patient profiles, healthcare professionals can enhance adherence to care strategies, ultimately supporting better health outcomes.
Moreover, managing blood sugar is a shared journey. Building a supportive community can greatly enhance this experience. T2DSolutions serves as a crucial resource center for individuals navigating blood sugar regulation, offering educational materials and community support tailored for those recently diagnosed. For instance, case studies such as the two-step strategy for gestational diabetes mellitus (GDM) screening illustrate the effectiveness of personalized methods in managing glucose levels.
This approach has been shown to reduce neonatal complications without increasing the risk of small-for-gestational-age births, underlining the potential benefits of customized treatment plans across various contexts. As R.M.B. wisely points out, "Customized treatment strategies are crucial for effective control of blood sugar levels, as they consider the unique circumstances of each patient."
As the field of blood sugar care continues to evolve, integrating insights from A1C and average glucose measurements will be essential in crafting effective, personalized strategies. T2DSolutions is dedicated to supporting patients every step of the way on this journey.
The Role of Technology in Monitoring A1C and Average Glucose Levels
Technology is transforming diabetes care, especially in how we track A1C versus average glucose levels. Continuous glucose monitors (CGMs) are at the forefront of this change, offering real-time insights into blood sugar fluctuations. This immediate feedback empowers you to make informed decisions about your diet and medication, significantly enhancing your ability to manage your condition effectively.
It's understandable to feel overwhelmed, but studies show that even short interventions lasting less than three months can lead to notable improvements in body mass index (BMI), with a mean difference of -3.06 (95% CI -5.65 to -0.47; p=0.02). This highlights the potential of timely data to positively influence your health outcomes.
Mobile applications complement CGMs by monitoring A1C results and providing insights into A1C versus average glucose levels. These apps offer valuable reminders that support improved management. By embracing these technological advancements, you not only enhance the precision of your blood sugar monitoring but also take a proactive role in your health journey. Many patients using CGMs alongside mobile applications report better adherence to treatment plans and a deeper understanding of their sugar patterns, which can lead to improved overall health outcomes.
Experts emphasize the crucial role technology plays in blood sugar control. Continuous glucose monitors have been shown to enhance care outcomes for those managing blood sugar issues by providing consistent and reliable data. This information is essential for tracking A1C versus average glucose levels. As the landscape of glucose condition oversight evolves, the integration of technology continues to support you on your journey, fostering a collaborative approach to health that emphasizes shared knowledge and community support.
Case studies, including the Cochrane Risk-of-Bias Tool Assessment, demonstrate a significant decrease in the likelihood of complications, further confirming the importance of these technologies in modern health management. As Laura Wood, Senior Press Manager, notes, "For more information about this report visit https://researchandmarkets.com/r/fyih08." You're not alone in this journey; we are here to support you every step of the way.

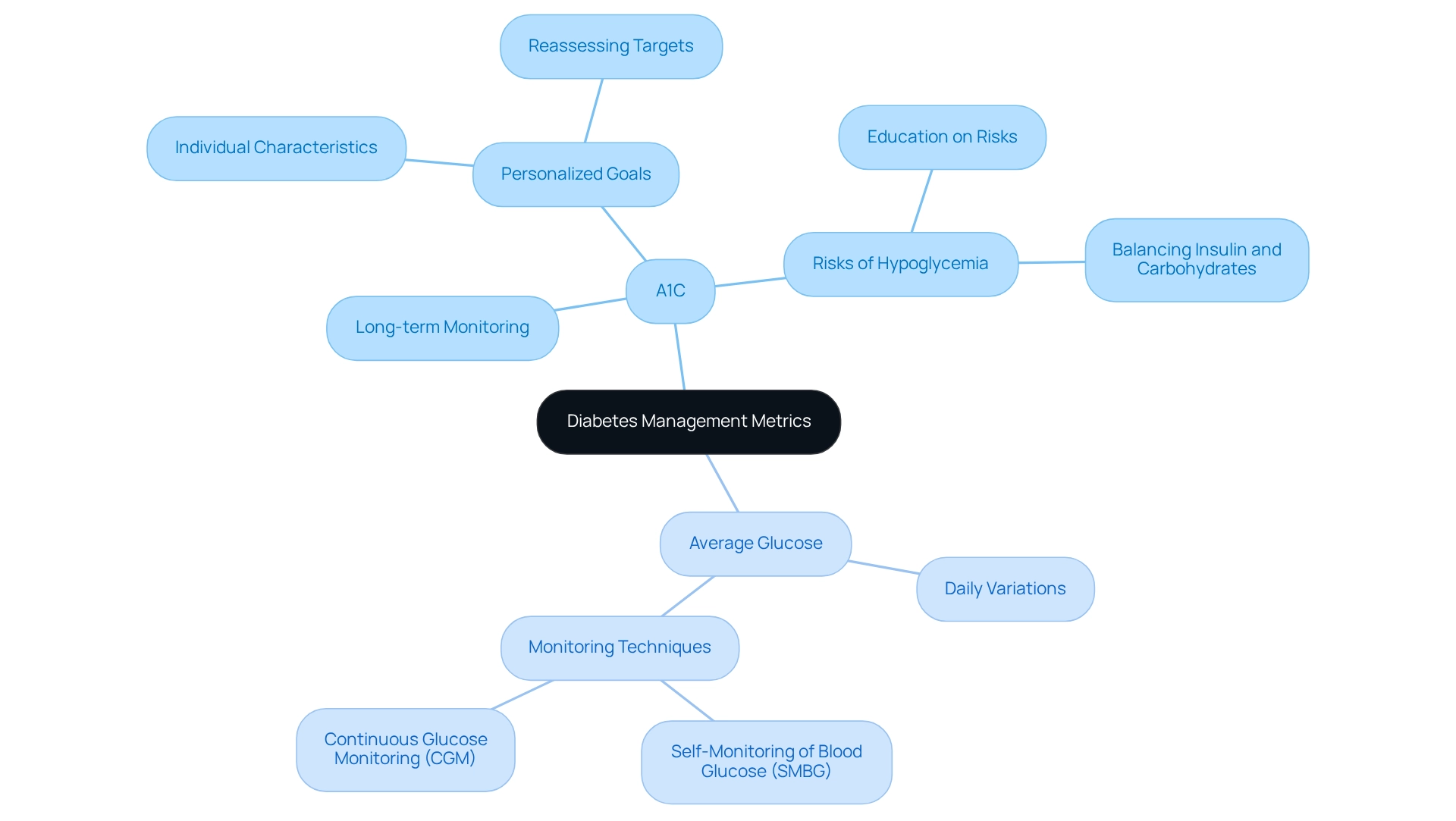
Key Takeaways: A1C vs Average Glucose in Diabetes Management
Understanding A1C versus average glucose is essential for managing your health. Both metrics serve important roles in comprehending sugar regulation, each offering unique insights into your condition. While A1C provides a long-term view of blood sugar levels over the past two to three months, average glucose captures daily fluctuations that can significantly impact your well-being.
At T2DSolutions, we recognize how vital these metrics are in managing blood sugar conditions. Grasping the relationship between A1C and average glucose is crucial for tailoring your management plan. The American Diabetes Association (ADA) highlights the importance of personalizing glycemic targets based on individual characteristics, such as life expectancy and other health concerns.
This personalized approach allows healthcare professionals to set realistic goals that balance the risks of hypoglycemia with the benefits of effective blood sugar management, particularly for those with a long-standing condition or multiple health issues. A case study titled "Setting and Modifying A1C Goals" illustrates how individualized targets can lead to improved health outcomes.
Recent studies indicate that individuals with diabetes face a higher risk of complications, such as hospitalization due to infections or dehydration, compared to those without the condition. This underscores the importance of consistent blood sugar monitoring. Self-monitoring of blood sugar (SMBG) is crucial for those on insulin, while continuous glucose monitoring (CGM) is becoming a valuable complementary tool. As noted in recent findings, "In conclusion, our research emphasizes the significance of taking into account both HbA1c and GMI in overseeing conditions related to blood sugar, particularly for individuals using CGM," shared Andre E. Manov, a supervision expert.
Healthcare experts emphasize that monitoring A1C and average glucose is vital in caring for those with blood sugar issues. Understanding these metrics empowers you to manage your health effectively. By integrating both A1C and average glucose into your personalized care strategy, you can achieve better health outcomes and enhance your quality of life.
At T2DSolutions, we are committed to providing resources and support for your health journey. Here are some key takeaways for effective diabetes management in 2025:
- Regularly monitor both A1C and average glucose to understand overall control and daily variations.
- Educate yourself on situations that increase the risk of hypoglycemia and the importance of balancing insulin and carbohydrate intake.
- Continuously reassess your glycemic targets to adapt to changing health conditions and treatment responses.
In conclusion, understanding A1C versus average glucose is crucial for informed decision-making in managing blood sugar levels. This knowledge empowers you to navigate your health journey with confidence. We invite you to subscribe to T2DSolutions for ongoing updates and resources that can support your diabetes management.
Conclusion
Understanding the relationship between A1C and average glucose is crucial for effective diabetes management. A1C serves as a long-term measure, reflecting average blood sugar levels over the past two to three months, while average glucose provides insights into daily fluctuations. Both metrics are essential in developing personalized treatment plans that cater to individual patient needs, ultimately leading to improved health outcomes.
As diabetes care continues to evolve, integrating these measurements with advancements in technology—such as continuous glucose monitors and mobile applications—empowers you to take an active role in managing your condition. It's understandable to feel overwhelmed, but this proactive approach not only enhances your understanding but also fosters greater engagement in your management journey, which is vital for achieving a better quality of life.
In summary, the interplay between A1C and average glucose is not just about numbers; it’s about creating a comprehensive and personalized strategy for diabetes management. By regularly monitoring and interpreting these metrics, you can navigate your health journey with confidence and make informed decisions that positively impact your overall well-being. Remember, access to resources and support, like those provided by T2DSolutions, is essential in this journey, ensuring that you have the tools you need to thrive in your diabetes management. You're not alone in this journey, and we are here to support you every step of the way.
Frequently Asked Questions
What is A1C and why is it important?
A1C, or glycated hemoglobin, is a blood test that measures the percentage of hemoglobin molecules with sugar attached, reflecting average glucose levels over the past two to three months. It is crucial for diagnosing diabetes and assessing treatment effectiveness.
How does A1C compare to average blood sugar levels?
A1C provides a long-term view of blood sugar regulation, while average blood sugar offers immediate insights into daily fluctuations. Both metrics are essential for managing blood sugar levels effectively.
What do different A1C levels indicate?
An A1C level below 5.7% is normal, 5.7% to 6.4% indicates prediabetes, and 6.5% or higher confirms diabetes. Understanding these thresholds helps gauge risk and the need for lifestyle or medical interventions.
How often should A1C testing be conducted?
It is estimated that by 2025, about 70% of individuals with high blood sugar will undergo A1C testing at least twice a year, highlighting its significance in ongoing healthcare.
What is the relationship between A1C and average glucose levels?
Average glucose levels can be estimated from A1C results using the formula: eAG (estimated average sugar) = (28.7 × A1C) - 46.7. This helps patients connect lab results with daily blood sugar monitoring.
Why is maintaining average glucose levels important?
Research shows that keeping average glucose levels below 154 mg/dL can significantly reduce the risk of diabetes-related complications, empowering patients to set realistic health goals.
What factors can affect blood sugar levels in a hospital setting?
Factors include previous hypoglycemic occurrences, chronic kidney disease, and irregular eating habits, which make controlling blood sugar levels more challenging in various environments.
How can stress impact blood sugar regulation?
Chronic stress can negatively affect metabolic functions, including blood sugar regulation. Managing stress through activities like yoga and counseling can improve overall health outcomes.
What resources does T2DSolutions provide for diabetes management?
T2DSolutions offers educational materials, community support, case studies, and expert insights to help patients understand and manage their A1C and average blood sugar levels effectively.
How can patients best utilize A1C and average glucose metrics in their diabetes management?
By learning to calculate and interpret A1C and average glucose values, patients can take proactive steps toward better health and quality of life, supported by resources from T2DSolutions.
