Overview
This article highlights the importance of understanding and applying ICD-10 codes for diabetes screening. It focuses on the top ten codes that healthcare professionals should know, ensuring effective patient management. Accurate coding is essential, as it not only aids in early diagnosis and intervention but also influences healthcare costs and reimbursement processes. By improving care coordination and management strategies, we can enhance overall patient outcomes.
It's understandable to feel overwhelmed by the complexities of coding. However, knowing the right codes can make a significant difference in your healthcare journey. We encourage healthcare professionals to familiarize themselves with these codes, as it empowers them to provide the best possible care for their patients. Remember, you’re not alone in this process; there are resources available to support you.
By focusing on accurate coding, we can work together to ensure that patients receive timely interventions and appropriate care. This not only helps in managing diabetes effectively but also fosters a sense of community and support among healthcare providers and patients alike. We are here to support you every step of the way.
Introduction
In the realm of healthcare, the significance of accurate coding cannot be overstated, especially when managing chronic conditions like diabetes. It's understandable to feel overwhelmed by the complexities of healthcare, but the ICD-10 coding system serves as a vital tool for healthcare providers. It enables them to classify diagnoses, symptoms, and procedures with precision, ensuring that you receive the care you deserve.
This article delves into the critical role of ICD-10 codes in diabetes screening. By understanding these codes, you can facilitate timely interventions and enhance your health outcomes. As the prevalence of diabetes continues to rise, grasping the importance of these codes becomes essential—not only for effective treatment but also for ensuring proper insurance reimbursements and guiding public health initiatives.
We aim to empower healthcare professionals and patients alike to navigate the complexities of diabetes management effectively. By exploring the latest updates and best practices in coding, we hope to support you every step of the way. Remember, you're not alone in this journey; we are here to provide the information and resources you need.
Understanding ICD-10 Codes: A Key to Diabetes Screening
ICD-10 classifications are a vital standardized system for categorizing and labeling diagnoses, symptoms, and procedures, particularly for screening diabetes ICD 10. These classifications empower healthcare professionals to identify individuals at risk, ensuring they receive timely and appropriate care. Understanding these codes is essential not only for accurate documentation and billing but also for improving patient outcomes through better care coordination.
As we look ahead to 2025, the importance of screening diabetes ICD 10 codes in managing diabetes-related conditions is paramount. They play a crucial role in facilitating effective screening, which is vital for early intervention and management. Recent statistics reveal that medical costs associated with diabetes have risen from $10,179 to $12,022 per person between 2012 and 2022. This increase highlights the financial burden of unmanaged health issues and underscores the necessity for accurate coding to help alleviate these costs.
The STUDY for Diabetes in Youth, tracking youth-onset conditions since 2001, emphasizes the impact of ICD-10 classifications on screening diabetes ICD 10 for the illness. This extensive research provides valuable insights into the incidence and prevalence of diabetes among young individuals, highlighting the need for accurate classification and surveillance for effective management. The findings from such studies reinforce the significance of screening diabetes ICD 10 classifications in understanding trends in blood sugar conditions and enhancing patient outcomes.
Moreover, recent evaluations show that the sensitivity of physician claims-based case definitions for diabetes has improved over time, indicating a growing recognition of the importance of precise classification. However, there has been a slight decrease in specificity and positive predictive value (PPV), which suggests the need for ongoing education and training for healthcare providers in applying these classifications.
As Jean M Lawrence from the Department of Research and Evaluation at Kaiser Permanente Southern California states, "Accurate coding, particularly screening diabetes ICD 10, is essential for effective management of the condition and can significantly influence care outcomes." This expert perspective further underscores the importance of screening diabetes ICD 10 classifications in the context of glucose monitoring. These classifications not only enhance care management but also support public health initiatives aimed at preventing health issues.
By ensuring that healthcare providers are well-informed about these systems, we can improve the quality of care provided to individuals, ultimately leading to better health outcomes.
At T2DSolutions, we recognize the essential role that precise screening diabetes ICD 10 plays in managing diabetes-related conditions. Our platform is dedicated to equipping newly diagnosed patients with the resources and education necessary to understand these codes and their implications for health. Real-world examples illustrate how effective ICD-10 classification can lead to improved management of blood sugar conditions.
For instance, healthcare systems that have embraced thorough classification practices report higher rates of early diagnosis and intervention, which are crucial for preventing complications associated with blood sugar disorders. As we move forward, maintaining a strong focus on accurate ICD-10 coding will be vital in shaping the future of care and management for diabetes.
Top 10 ICD-10 Codes for Diabetes Screening
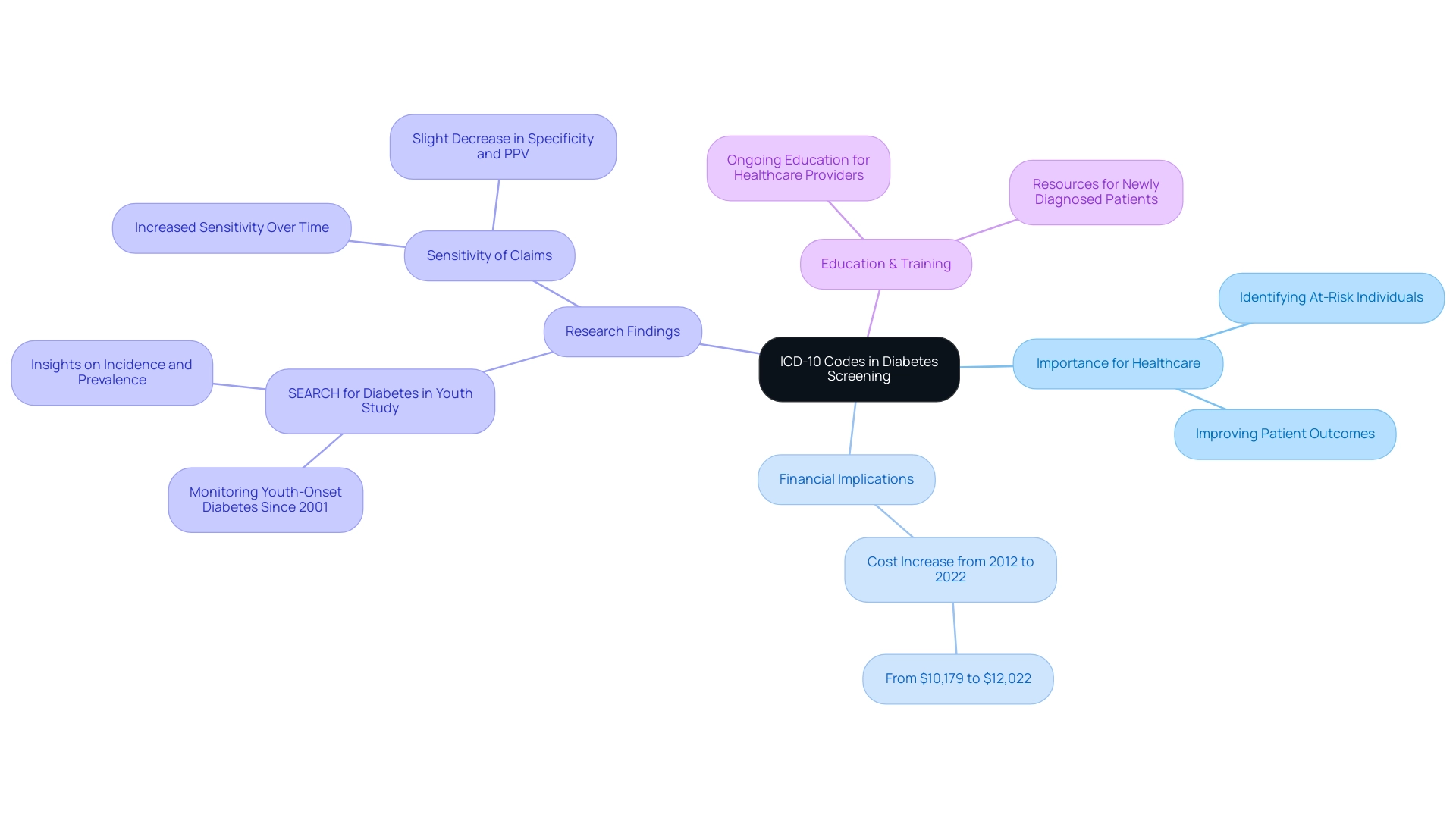
At T2DSolutions, we are deeply committed to providing extensive resources for the education and management of blood sugar conditions. Understanding the ICD-10 classifications is crucial for effectively screening and managing these disorders. Here are some important classifications to keep in mind:
- Z13.1: Encounter for screening for blood sugar disorders. This program is essential for identifying patients who need screening for high blood sugar, enabling early detection and management.
- E11.9: Type 2 high blood sugar mellitus without complications. This script is frequently utilized to record instances of Type 2 mellitus that do not show any immediate complications, allowing for effective monitoring and treatment.
- E10.9: Type 1 mellitus without complications. Similar to E11.9, this identifier is crucial for recording Type 1 cases without complications, ensuring suitable care pathways are adhered to.
- E13.9: Other specified mellitus without complications. This program identifies different types of blood sugar conditions that do not fit into the more prevalent categories, assisting in thorough management of individuals.
- R73.9: Hyperglycemia, unspecified. This guideline is applied when a patient shows elevated blood sugar levels but lacks a confirmed diagnosis of glucose intolerance, necessitating further examination.
- R73.03: Prediabetes. This program is essential for recognizing individuals at risk of developing the illness, enabling early intervention strategies to be executed.
- E11.65: Type 2 diabetes mellitus with hyperglycemia. This script signifies instances where Type 2 mellitus is accompanied by high blood sugar levels, necessitating more intensive management.
- E10.65: Type 1 mellitus with hyperglycemia. Similar to E11.65, this designation is used for Type 1 cases with hyperglycemia, emphasizing the necessity for careful monitoring and treatment modifications.
- E11.8: Type 2 mellitus with other specified complications. This script is crucial for recording Type 2 conditions that involve complications, ensuring that comprehensive care is provided.
- E10.8: Type 1 mellitus with other specified complications. This programming serves a similar function for Type 1 conditions, enabling healthcare providers to manage any complications effectively.
These ICD-10 classifications are vital for accurately recording screening diabetes ICD 10 and ensuring suitable follow-up care. Recent studies indicate that 33.4% of adults aged 40 to 70 with overweight or obesity received blood glucose testing, a figure that rose to 74.3% when including various glucose measures. Additionally, 70.8% of U.S. adults with diagnosed conditions had elevated blood pressure, underscoring the broader health implications of managing this illness.
The application of screening diabetes ICD 10 classifications aids swift and economical monitoring of blood sugar disorders, in contrast to conventional active monitoring techniques. Starting in 2025, remaining informed about these regulations is essential for healthcare professionals to guarantee effective management of blood sugar conditions and patient care. The findings from the study on testing prevalence could inform clinical and public health efforts to improve screening for blood glucose levels among adults with overweight or obesity.
JML reports grants from the Centers for Disease Control and Prevention during the conduct of the study, further emphasizing the importance of these codes in enhancing screening practices. For additional resources and updates on blood sugar management, we encourage you to subscribe to T2 Solutions. Remember, you're not alone in this journey; we are here to support you every step of the way.
The Importance of Accurate Coding in Diabetes Management
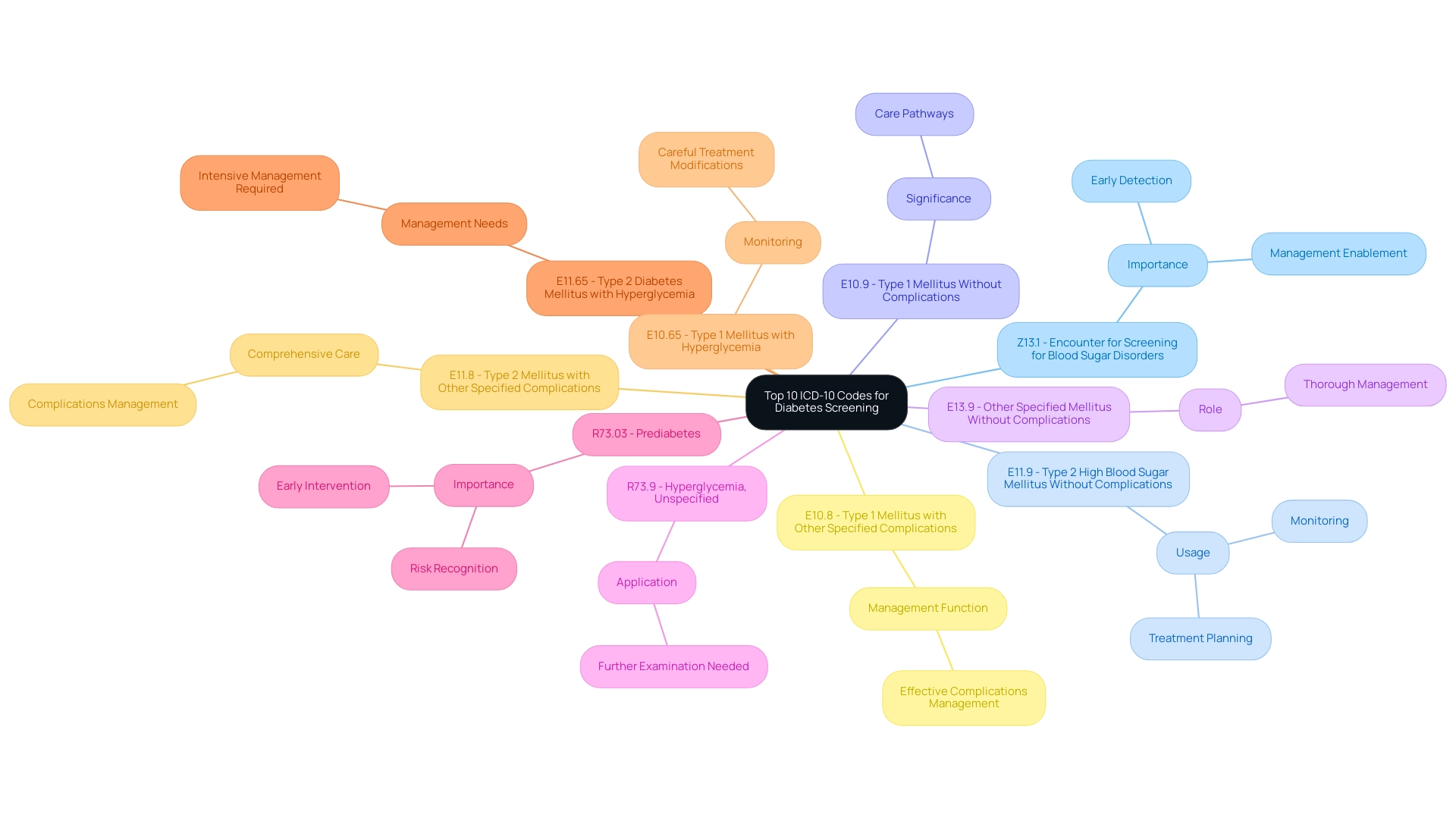
Managing blood sugar levels with precision is crucial for effective communication among healthcare providers regarding an individual's condition and treatment needs. It lays the groundwork for securing insurance reimbursements and advancing research into diabetes trends. When programming is incorrect, it can lead to misclassification, resulting in treatment plans that may not suit individual needs and can adversely affect health outcomes.
For instance, a recent study highlighted that the glycemic control group faced an alarming 42.2% error rate, emphasizing the necessity for accuracy in this area. Such high error rates can cause significant delays in receiving appropriate care, ultimately affecting the overall health and well-being of individuals.
Healthcare providers are increasingly recognizing the importance of precise classification in enhancing care for individuals. By embracing strong programming practices, they can develop treatment plans tailored to individual needs. For example, the iCare Mobile Diabetes Management Program demonstrated that individuals who adhered closely to protocols experienced noteworthy improvements in their ABC levels—hemoglobin A1c, blood pressure, and low-density lipoprotein cholesterol—over a 12-month period.
This illustrates how precise documentation directly correlates with better diabetes management outcomes and reinforces the necessity for healthcare professionals to prioritize accuracy in their records.
Moreover, precise programming is not just an administrative concern; it has tangible effects on treatment strategies and individual outcomes. Experts in the field note, "The longer the active use of the application at a high compliance level, the higher the possibility that the target ABC level was achieved." This connection highlights the critical role of programming in monitoring patient progress and ensuring treatment strategies align effectively with health goals.
When it comes to insurance reimbursement, statistics reveal that accuracy in classification is vital. Errors in programming can lead to rejected claims, impacting the financial sustainability of blood sugar management initiatives. Additionally, privacy protection measures were put in place during studies to safeguard confidentiality, enhancing the credibility of the findings.
As a result, healthcare practitioners must focus on precision in coding to improve holistic care and health outcomes for those they serve. Community involvement and support are also essential components of effective management, aligning with T2DSolutions' mission to empower individuals and families on their health journeys. T2DSolutions serves as a valuable resource center, providing education and support for those newly diagnosed as they navigate their condition.
Impact of ICD-10 Coding on Patient Care and Insurance
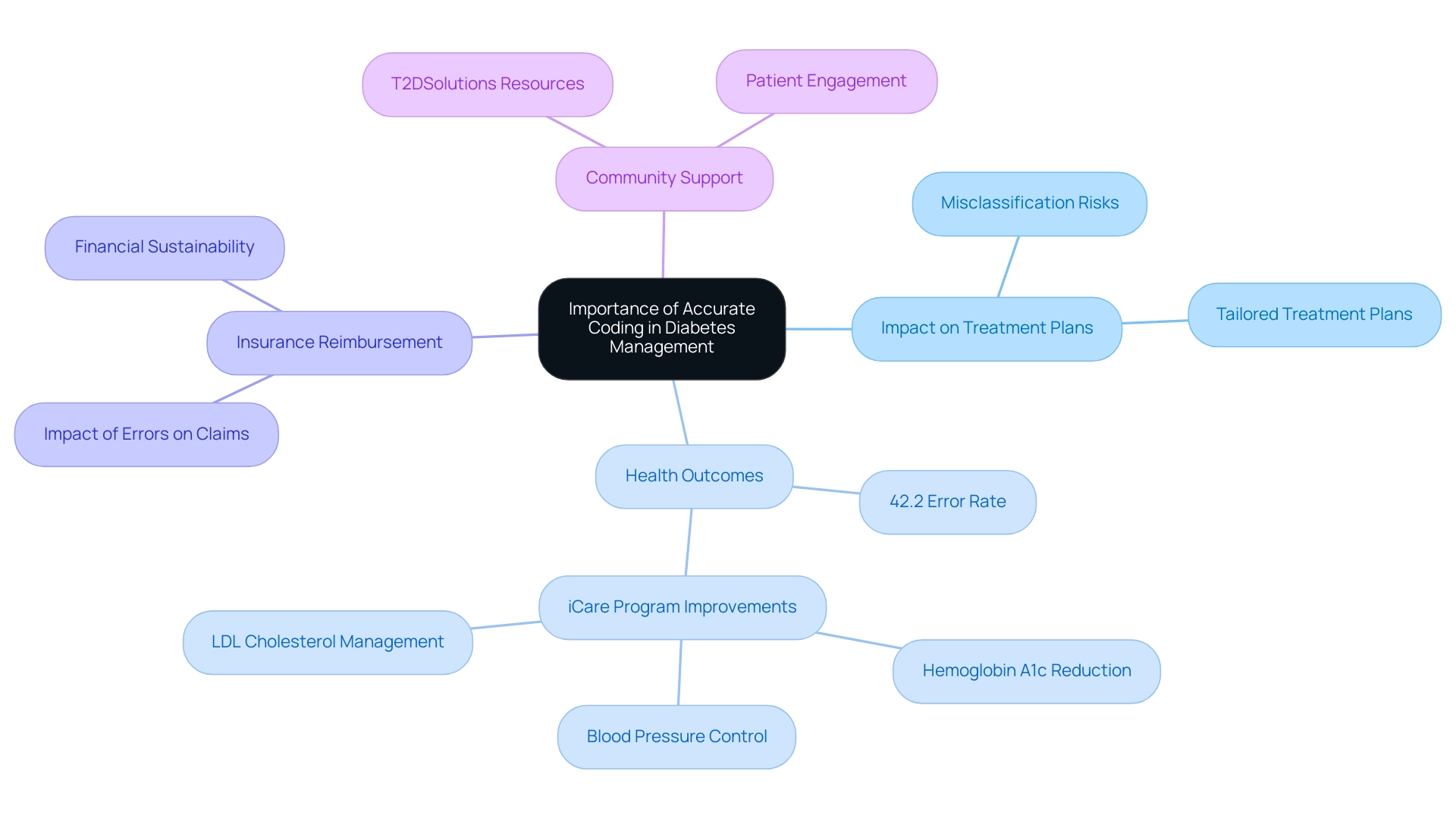
ICD-10 classification plays a crucial role in diabetes care, providing healthcare providers with the vital information needed to make informed clinical decisions. This precise programming not only facilitates timely interventions and the development of appropriate treatment plans but also significantly impacts insurance reimbursement processes. Mistakes in programming can lead to claim denials or delays, threatening the financial stability of healthcare practices and ultimately influencing access to essential care.
In 2025, the connection between programming accuracy and insurance reimbursement has become increasingly evident. Hospitals have reported an overall average accuracy of 91.3% over a 12-month monitoring period, highlighting the importance of precise documentation in ensuring that patients receive the care they need without unnecessary financial barriers. It’s encouraging to note that every nine months, a new group of hospitals is integrated, contributing to ongoing enhancements in documentation practices.
However, challenges persist. Recent surveys indicate that periodic training and the hiring of additional staff are essential to enhance practices and reduce errors. Yasir Abdelgadir noted, "While effective for initial single-identifier scenarios, we recognize the need for strategies to handle new identifiers and more complex, multi-identifier situations."
Case studies further demonstrate the relationship between ICD-10 classification and screening diabetes ICD 10 in healthcare management. One notable study assessed the performance of AI tools like ChatGPT in nephrology classification, comparing its outputs against a standard set of correct ICD-10 codes. This research highlights the potential for technology to improve accuracy in programming, which is crucial for effective patient management.
Moreover, the effect of programming accuracy extends to insurance claim denial rates. Mistakes in programming can lead to significant delays in reimbursement, hindering healthcare providers' ability to deliver timely care. As healthcare professionals navigate the complexities of managing chronic conditions, understanding the nuances of ICD-10 classification becomes essential—not only for ensuring compliance but also for optimizing outcomes for individuals and maintaining the financial health of their practices.
In summary, the impact of screening diabetes ICD 10 classification on care for individuals with blood sugar issues is profound, affecting everything from treatment strategies to insurance reimbursements. As the terrain of healthcare continues to evolve, remaining knowledgeable about billing practices will empower both providers and patients to tackle the difficulties of managing health conditions effectively. Remember, you’re not alone in this journey; we are here to support you every step of the way.
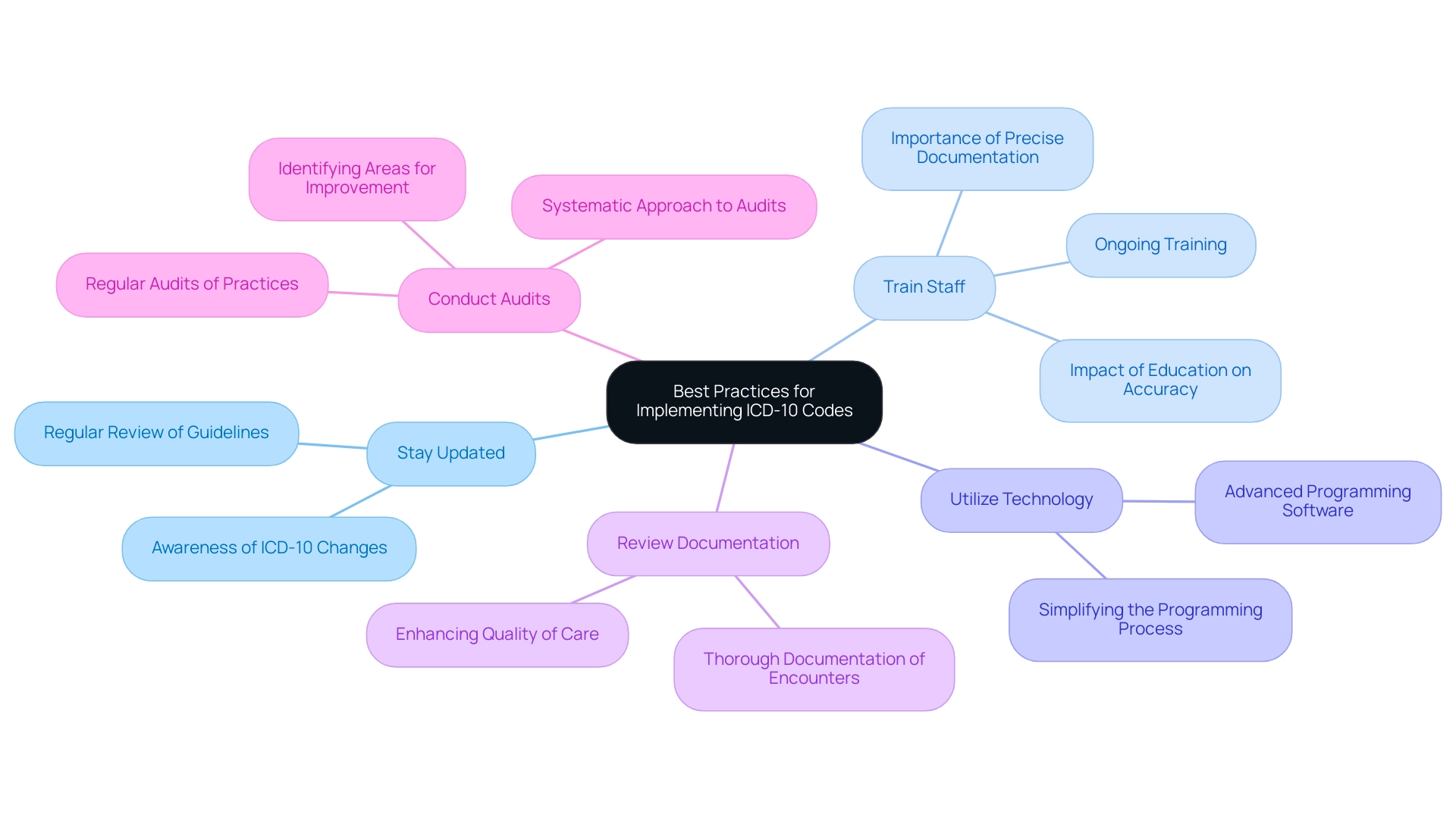
Best Practices for Implementing ICD-10 Codes in Clinical Settings
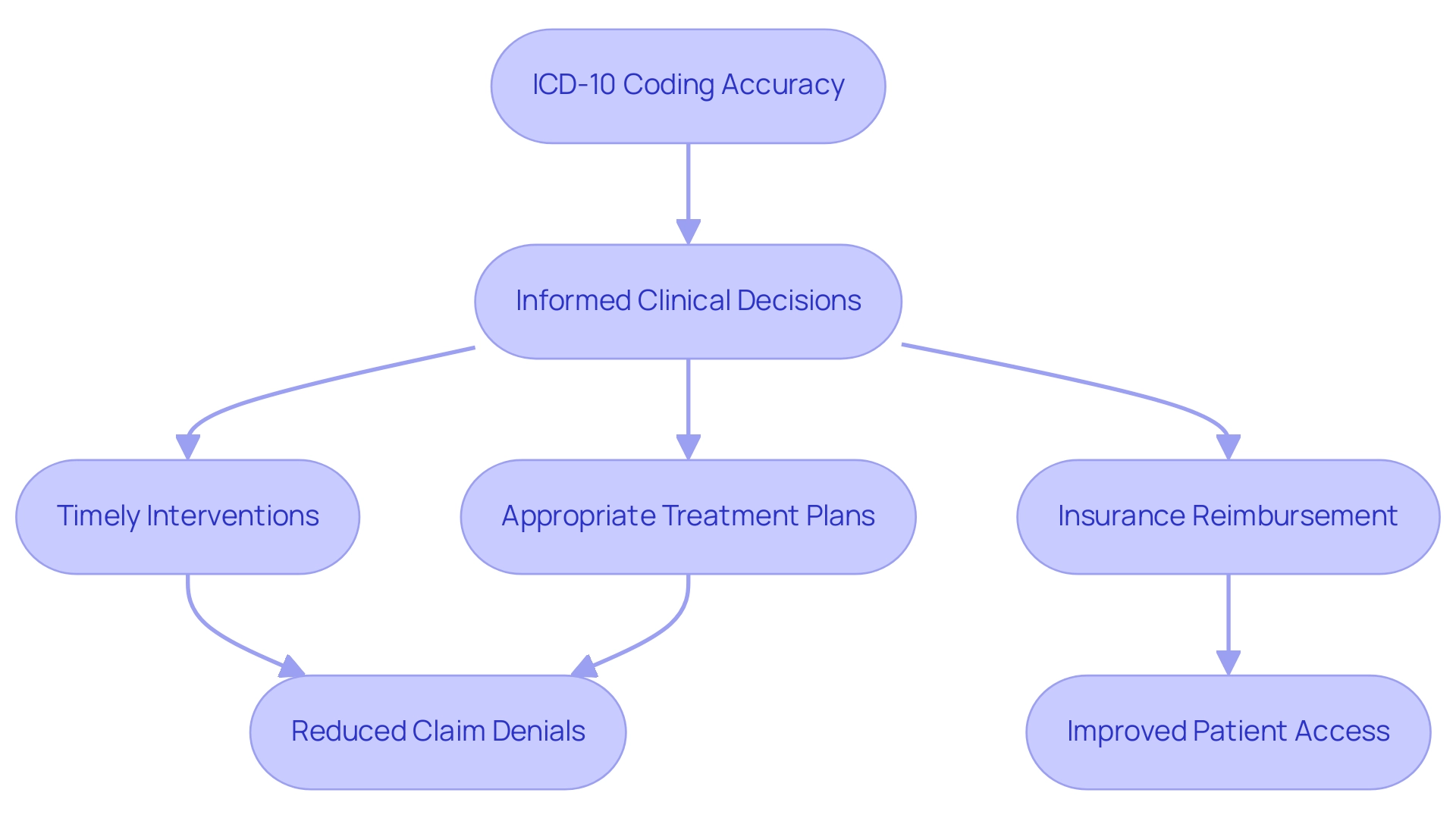
Stay Updated: It's important to regularly review programming updates and guidelines. This helps ensure that you are compliant with the latest standards. Staying informed about changes in ICD-10 codes, particularly those related to screening for diabetes, is essential as the classification landscape continually evolves.
Train Staff: Ongoing training for your team is crucial. It emphasizes the importance of precise documentation, which can feel overwhelming at times. Research shows that effective training programs significantly enhance coders' knowledge and skills, leading to improved programming accuracy. Santos observed that a lack of ongoing education for clinical coders can impact the accuracy, completeness, and timeliness of classification. Facilities that prioritize continuous education for their clinical coders often report better performance outcomes.
Utilize Technology: Implementing advanced programming software can be a game changer. These tools help recognize the appropriate identifiers based on clinical documentation, simplifying the programming process and reducing mistakes. This allows healthcare providers to focus more on what truly matters—client care.
Review Documentation: It's vital to ensure that all encounters are thoroughly documented. This not only supports the selected codes but also enhances the overall quality of care by providing a clear clinical picture.
Conduct Audits: Regular audits of programming practices are important for identifying areas where improvement is needed. Facilities that conduct routine audits often find that they can enhance their documentation processes, leading to better compliance and improved patient outcomes. A recent study concluded that continuous education and training for clinical coders are essential for enhancing the quality of coded data in healthcare environments. This reinforces the need for a systematic approach to audits. Furthermore, the findings support the importance of effective training programs that enhance coders' knowledge and skills, ensuring that the programming process remains accurate and efficient. You're not alone in this journey; we are here to support you every step of the way.
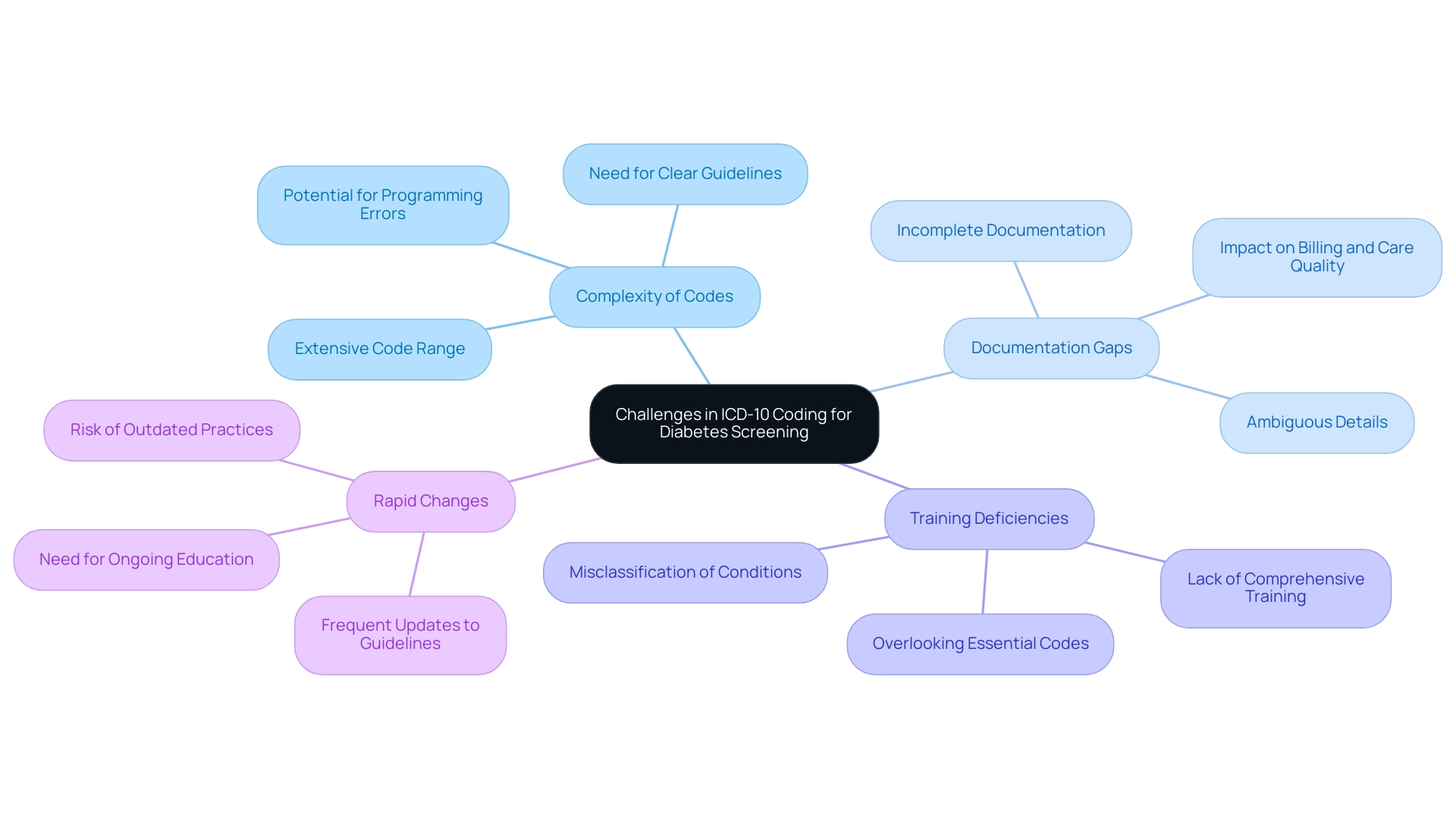
Challenges in ICD-10 Coding for Diabetes Screening
Navigating the classification of screening diabetes ICD-10 can be a daunting experience. It's understandable to feel overwhelmed by the challenges that arise, as these multifaceted issues can significantly impact the accuracy of patient records and care outcomes. Let’s explore some common hurdles together:
-
Complexity of Codes: The ICD-10 classification system is extensive, encompassing a wide array of codes. This complexity can lead to confusion among healthcare providers, resulting in potential programming errors. Clear guidelines and resources are essential to help navigate this intricate landscape.
-
Documentation Gaps: Incomplete or ambiguous documentation can hinder accurate programming. When healthcare providers miss capturing necessary details in medical records, it can lead to misclassification of diabetes types or missed diagnoses altogether. This not only affects billing but also the quality of care you receive during screening.
-
Training Deficiencies: A lack of comprehensive training among healthcare staff may contribute to significant classification errors. Without adequate instruction on the intricacies of ICD-10 codes, providers might misclassify conditions or overlook essential codes, resulting in discrepancies in individual data.
-
Rapid Changes: The healthcare landscape is continually evolving, with frequent updates to classification guidelines. It's crucial for healthcare providers to engage in ongoing education and adaptation to stay current. Falling behind can lead to outdated practices that compromise accuracy.
Addressing these challenges is vital for enhancing accuracy in the screening diabetes ICD-10 process and ultimately improving your care. For instance, a recent study titled 'Collaborative Solutions for ICD-10 Discontinuities' highlighted the importance of collaborative solutions to tackle documentation gaps. It suggested establishing a web-based platform for sharing best practices among providers. Such initiatives can foster a community strategy to overcome these obstacles, ensuring healthcare professionals are equipped with the knowledge and tools essential for effectively managing diabetes-related issues.
Statistics show that documentation gaps greatly impact accuracy in reporting, with many providers facing difficulties aligning their practices with the latest ICD-10 standards. As Stephanie Tomlin observed, 'Precise documentation is crucial for efficient management of diabetes-related conditions, and teamwork among healthcare professionals can lead to better results.' By focusing on training and community cooperation, healthcare providers can reduce these common errors and enhance the overall quality of care for individuals with blood sugar conditions. Moreover, the continuous need for revising computer scripts for analyzing ICD classifications underscores the importance of adapting to the latest standards to ensure precise practices. Remember, you're not alone in this journey; support is available to help you navigate these complexities.
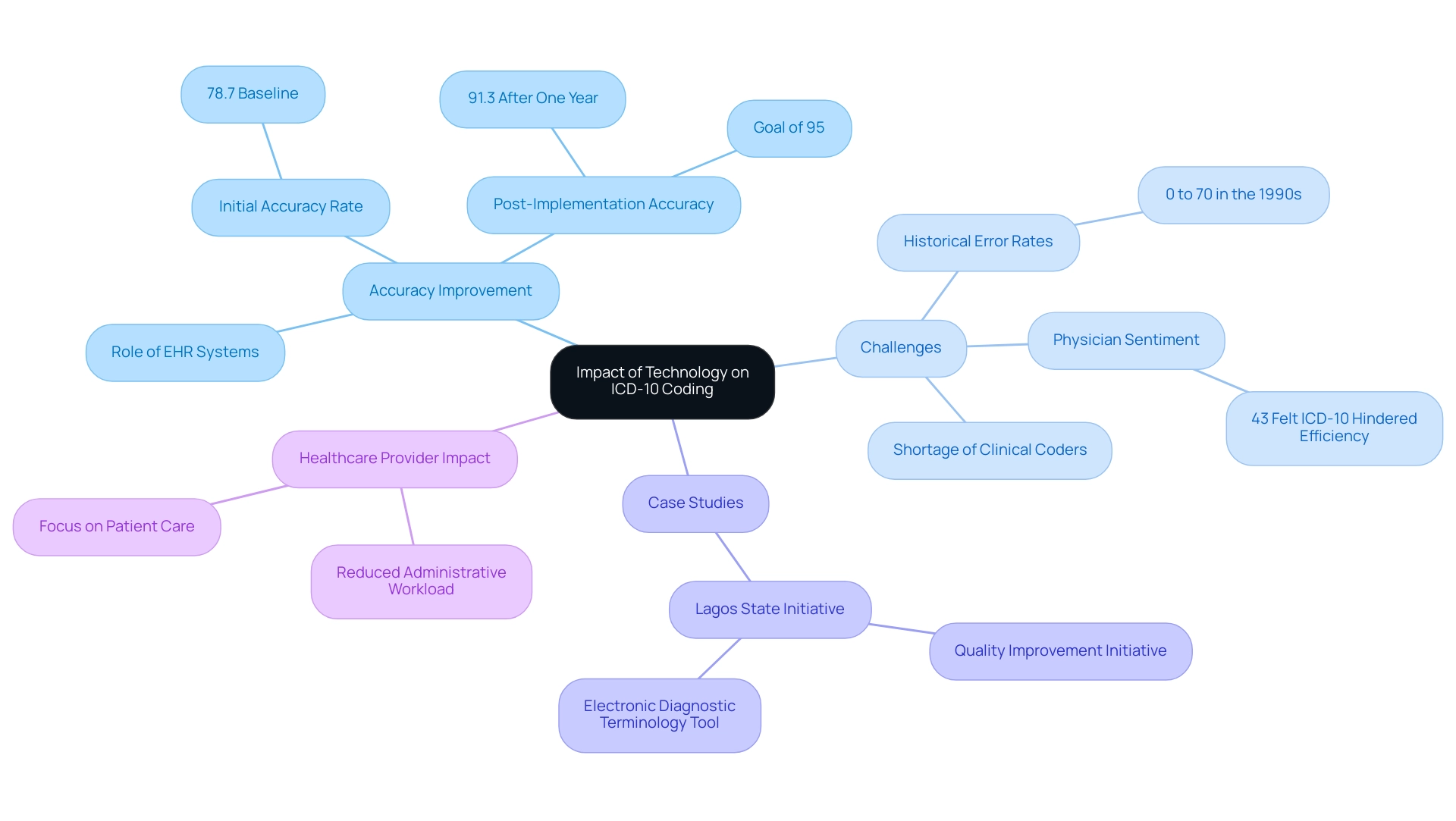
Leveraging Technology for Accurate ICD-10 Coding
Technology plays a vital role in improving the accuracy of screening for diabetes ICD-10 classification, especially in managing diabetes effectively. Electronic health records (EHR) and advanced software empower healthcare providers to select the right codes based on thorough clinical documentation. These tools not only simplify the programming process but also significantly minimize human error, which has historically affected accuracy, with error rates in the 1990s varying from 0 to 70 percent.
For instance, a quality enhancement initiative in Lagos State, Nigeria, showcased how implementing an electronic diagnostic terminology tool boosted accuracy from an initial 78.7% to an impressive 91.3% over just one year, with a goal of reaching at least 95%. This example illustrates the potential of technology to enhance reliability and efficiency in programming practices, particularly in resource-limited settings.
Moreover, the introduction of automated programming systems has been shown to ease the workload on healthcare workers, allowing them to focus more on patient care rather than administrative tasks. A survey indicated that 43% of physicians felt the transition to ICD-10 hindered practice efficiency, underscoring the need for effective technological solutions. By utilizing EHR systems, healthcare providers can ensure more accurate classification for screening diabetes ICD-10, leading to better patient outcomes and more efficient billing processes.
As T2DSolutions evolves into a new resource center for health education and community support, it recognizes the importance of precise classification in enhancing care management for individuals with blood sugar concerns. As Adenike Omosun from the Lagos State Ministry of Health emphasized, "Find articles by Adenike Omosun," highlighting the significance of ongoing research and development in this field. As we approach 2025, the role of technology in refining ICD-10 coding precision continues to progress, promising even greater advancements in care management. You're not alone in this journey, and we are here to support you every step of the way.
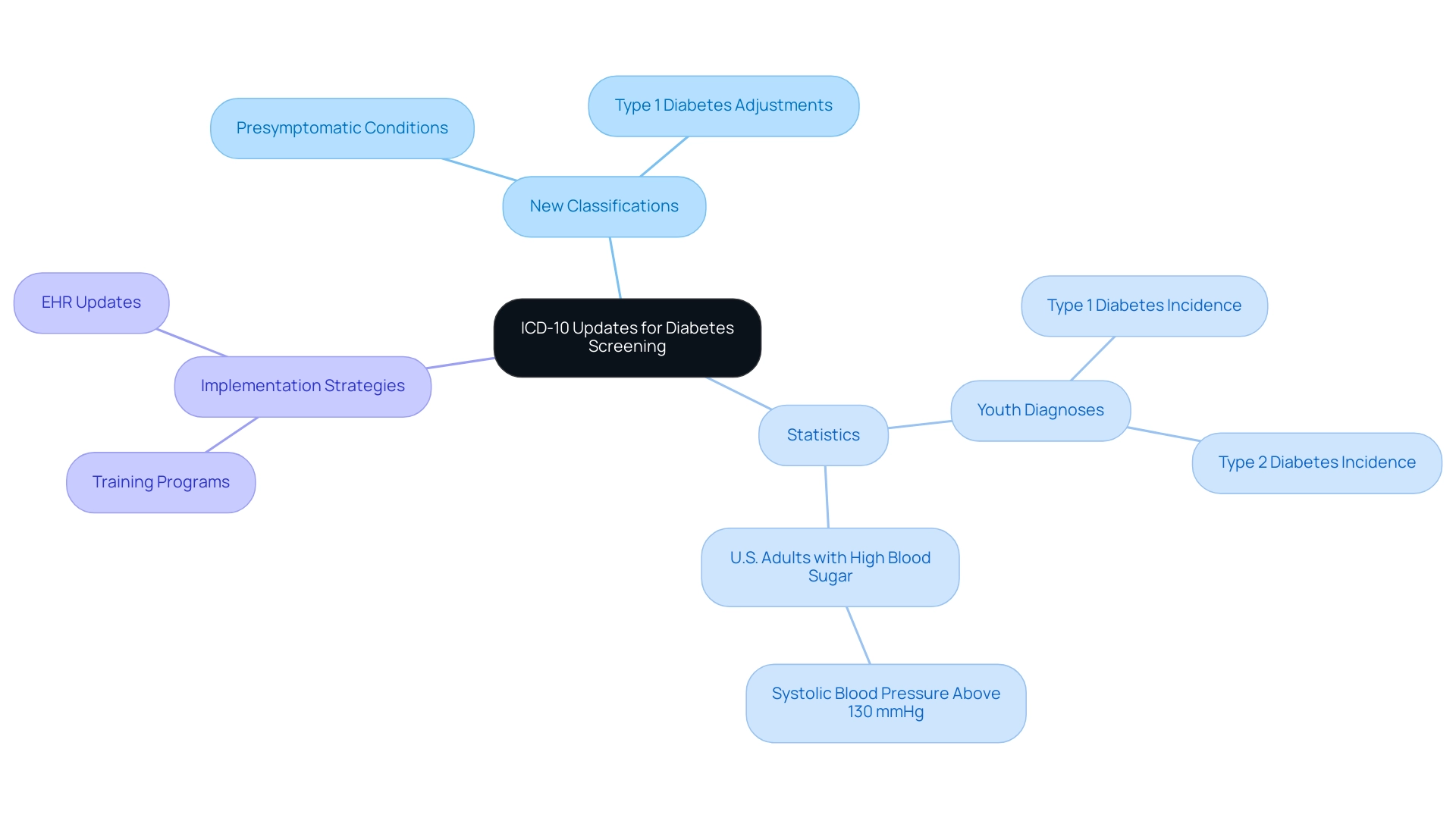
Recent Updates in ICD-10 Codes for Diabetes Screening
At T2DSolutions, we are deeply committed to enhancing care for individuals with diabetes. Recent updates to ICD-10 classifications for screening bring significant changes that improve the accuracy and specificity of diabetes diagnoses. These updates include new classifications for presymptomatic conditions and adjustments to existing classifications, ensuring that healthcare providers can better identify early-stage Type 1 diabetes. This is crucial for timely intervention and effective management, allowing patients to receive the care they need when they need it.
These updates respond to the rising occurrence of diabetes, especially among our youth. Recent studies reveal that during 2017-2018, around 5,293 children and adolescents were diagnosed with Type 2 diabetes. This statistic underscores the urgent need for effective screening and preventive measures tailored to younger populations. As the rates of diabetes continue to climb, precise documentation becomes increasingly important, directly impacting diagnosis rates and subsequent care strategies.
At T2DSolutions, we recognize the importance of adapting to these new ICD-10 codes. Our healthcare providers are implementing training programs and updating electronic health record systems to ensure compliance and enhance patient care. This proactive approach streamlines the programming process, supporting healthcare professionals in delivering more precise and effective treatment plans tailored to each patient's needs.
Expert opinions emphasize that these programming advancements are vital for improving health outcomes. S. Lee noted, "Our research offers insights on the precision of health condition classification among the NAFLD population, and similar methodologies can be utilized to evaluate other chronic conditions." This highlights how precise coding is critical for understanding broader implications and resource allocation in diabetes care.
Statistics reveal that 80.6% of U.S. adults with diagnosed conditions related to high blood sugar have a systolic blood pressure of 130 mmHg or above. This alarming figure highlights the urgent need for thorough management strategies, and the new classifications can play a significant role in promoting better health outcomes.
Overall, the recent updates to ICD-10 codes for diabetes screening reflect T2DSolutions' commitment to enhancing care through improved diagnostic accuracy. This ultimately benefits both individuals and healthcare providers alike. If you or someone you know has recently been diagnosed, we encourage you to subscribe to T2DSolutions for updates and resources that can support your diabetes management journey. Remember, you're not alone in this journey; we are here to support you every step of the way.
Staying Informed: Resources for ICD-10 Coding Updates
Healthcare professionals can effectively stay informed about ICD-10 coding updates through a variety of essential resources that support their journey in providing care:
-
Official Coding Guidelines: It’s important to regularly consult the Centers for Medicare & Medicaid Services (CMS) and the American Academy of Professional Coders (AAPC) websites. These platforms provide the latest coding guidelines and updates, which are crucial for precise programming practices. The CMS diagnosis-related group system includes 740 discrete classifications, highlighting the complexity of classification.
-
Professional Associations: Engaging with organizations like the American Diabetes Association (ADA) and the American Health Information Management Association (AHIMA) is vital. Membership in these associations opens doors to a wealth of resources, training opportunities, and networking that can enhance programming education and practices. As Stephanie Tomlin wisely observes, "Find articles by Jonathan Skinner," underscoring the importance of ongoing education in programming.
-
Webinars and Workshops: Actively participating in educational webinars and workshops focused on programming and diabetes management is an excellent way to stay current. These sessions often include expert insights and practical applications that can directly enhance accuracy in programming and patient care.
-
Programming Software: Implementing programming software that provides real-time updates on programming changes and guidelines can streamline the programming process. Such tools are invaluable for ensuring adherence to the latest standards and enhancing overall efficiency in programming practices.
-
Statistics on Resource Utilization: Recent data indicates that healthcare professionals increasingly rely on a mix of online resources, professional networks, and educational events to stay updated on ICD-10 modifications. This trend emphasizes the importance of continuous learning in the evolving landscape of healthcare.
-
Case Studies on ICD-10 Classification Education: For instance, Canadian researchers have developed a rigorous algorithm for translating ICD-9 to ICD-10 definitions, providing significant insights into the challenges of classification transitions. Their findings highlight the critical role of clinician judgment in refining definitions and improving health measurement accuracy. This case study illustrates the need for accurate translations and understanding of discontinuities for effective biostatistical modeling.
By utilizing these resources, healthcare professionals can deepen their understanding of ICD-10 classification, particularly in screening diabetes ICD-10. This ultimately leads to better management of blood sugar conditions and improved patient outcomes. Remember, the transition from ICD-9 to ICD-10 on October 1, 2015, was a pivotal moment in healthcare coding, making ongoing education and adaptation essential. You're not alone in this journey; we are here to support you every step of the way.
Key Takeaways for Effective Diabetes Screening Coding
-
Understanding the importance of ICD-10 classifications in screening for diabetes and managing blood sugar levels is crucial for effective healthcare. These codes not only enable accurate diagnoses but also play a vital role in tracking patient outcomes and ensuring healthcare providers receive appropriate reimbursement. For instance, in Ontario, a validated administrative data algorithm revealed that approximately 7.5% of the population was affected by diabetes in 2002. This statistic underscores the significance of precise programming in managing this widespread condition. As T2DSolutions launches, it aspires to be a key resource for newly diagnosed individuals, offering essential information on these classifications and their implications for care, along with tools like coding guides and access to expert consultations.
-
Familiarizing yourself with the primary ICD-10 classifications related to diabetes screening is essential. Codes such as E11 (Type 2 diabetes mellitus) and Z13.1 (encounter for screening for glucose regulation issues) are vital in identifying individuals who may need further evaluation and management. Effectively employing these systems can lead to improved care and outcomes for individuals. T2DSolutions will serve as an extensive resource, assisting you in navigating these critical aspects of diabetes management, with features like interactive tools and educational webinars.
-
Prioritizing accurate programming enhances healthcare and ensures appropriate compensation. A recent study highlighted that specific ICD-10 codes can effectively identify individuals with diabetic ketoacidosis (DKA) among those admitted to general internal medicine, although the accuracy varies by code. This variability highlights the necessity for healthcare providers to be meticulous in their documentation practices, helping to avoid misdiagnosis and ensuring patients receive the appropriate level of care. T2DSolutions will provide continuous updates and resources, including best practice guidelines and workshops, to support healthcare professionals in this important work.
-
In today’s rapidly changing healthcare environment, utilizing technology and resources to stay informed about programming practices is essential. Employing electronic health records (EHR) and classification software can simplify the classification process, reduce errors, and enhance the overall effectiveness of managing health conditions. T2DSolutions will offer insights and tools, such as a resource library for programming and access to programming experts, to help both patients and providers remain informed about the latest practices.
-
Ongoing training for you and your team on optimal methods for managing health conditions cannot be emphasized enough. Engaging in continuous training and workshops can significantly influence programming accuracy and, consequently, health screening results. For example, a participatory design project titled "Working Together to Improve Type 2 Care" demonstrated that collaboration between individuals with the condition and healthcare professionals led to actionable insights that enhanced Type 2 care. This illustrates the importance of user-centered design in healthcare, reinforcing the need for continuous learning and adaptation in programming practices. As Jean M Lawrence from the Department of Research and Evaluation at Kaiser Permanente Southern California states, "Continuous education in coding practices is essential for improving patient outcomes and ensuring effective diabetes management." T2DSolutions will be a vital partner in this educational journey, providing resources such as training modules and community forums.
Conclusion
Accurate ICD-10 coding is fundamental to effective diabetes screening and management. It plays a pivotal role in identifying patients at risk and facilitating timely interventions. By understanding and utilizing the relevant ICD-10 codes, healthcare providers can enhance patient outcomes and ensure appropriate reimbursement processes. The complexity of diabetes, coupled with rising prevalence rates, underscores the necessity for precise coding practices to avoid misclassification and ensure that patients receive the care they need.
Recent updates to the ICD-10 coding system reflect a commitment to improving diagnostic accuracy, particularly for emerging trends in diabetes among younger populations. These enhancements support healthcare providers in delivering effective treatment plans while contributing to broader public health initiatives aimed at diabetes prevention and management. As coding practices continue to evolve, integrating technology and ongoing education for healthcare professionals will be crucial in overcoming common challenges associated with coding accuracy.
Ultimately, prioritizing accurate ICD-10 coding is not merely an administrative task; it is an essential component of delivering high-quality healthcare. By leveraging available resources and committing to continuous learning, healthcare providers can navigate the complexities of diabetes management. This ensures that patients receive the best possible care. As the landscape of healthcare continues to change, staying informed and adaptable will empower both providers and patients in their journey toward better health outcomes. You're not alone in this journey, and together, we can work towards a healthier future.
Frequently Asked Questions
What is the purpose of ICD-10 classifications in healthcare?
ICD-10 classifications are a standardized system for categorizing and labeling diagnoses, symptoms, and procedures. They help healthcare professionals identify individuals at risk for conditions like diabetes, ensuring timely and appropriate care.
Why are screening diabetes ICD-10 codes important?
Screening diabetes ICD-10 codes are crucial for effective management of diabetes-related conditions. They facilitate early intervention and management, which is essential for improving patient outcomes and reducing healthcare costs associated with unmanaged diabetes.
What has recent research indicated about the financial implications of diabetes?
Recent statistics show that medical costs associated with diabetes have increased from $10,179 to $12,022 per person between 2012 and 2022, highlighting the financial burden of unmanaged diabetes and the necessity for accurate coding.
What insights does the STUDY for Diabetes in Youth provide regarding ICD-10 classifications?
The STUDY for Diabetes in Youth emphasizes the impact of ICD-10 classifications on understanding the incidence and prevalence of diabetes among young individuals, reinforcing the need for accurate classification and surveillance for effective management.
How has the sensitivity of physician claims-based case definitions for diabetes changed over time?
The sensitivity of physician claims-based case definitions for diabetes has improved, indicating a growing recognition of the importance of precise classification. However, there has been a slight decrease in specificity and positive predictive value (PPV), suggesting a need for ongoing education for healthcare providers.
What are some key ICD-10 classifications related to diabetes?
Important ICD-10 classifications for diabetes include: Z13.1: Encounter for screening for blood sugar disorders; E11.9: Type 2 diabetes mellitus without complications; E10.9: Type 1 diabetes mellitus without complications; E11.65: Type 2 diabetes mellitus with hyperglycemia; R73.03: Prediabetes.
What role does accurate ICD-10 coding play in diabetes management?
Accurate ICD-10 coding is essential for effective management of diabetes, influencing care outcomes, enabling tailored treatment plans, and securing insurance reimbursements. High error rates in coding can lead to misclassification and delays in appropriate care.
How does community support factor into diabetes management?
Community involvement and support are essential for effective diabetes management. Organizations like T2DSolutions provide education and resources to empower individuals and families in managing their health journeys.
What is the significance of ongoing education for healthcare providers regarding ICD-10 classifications?
Ongoing education for healthcare providers is vital to ensure they apply ICD-10 classifications accurately, which can improve patient care, enhance treatment strategies, and reduce errors that impact health outcomes and insurance reimbursements.
